- Infectious Diseases of Livestock
- Part 1
- Lesser known rickettsial infections in animals and humans
- Vectors: Ticks
- Vectors: Tsetse flies
- Vectors: Muscidae
- Vectors: Tabanidae
- Vectors: Culicoides spp.
- Vectors: Mosquitoes
- Classification, epidemiology and control of arthropod-borne viruses
- Special factors affecting the control of livestock diseases in sub-Saharan Africa
- The control of infectious diseases of livestock: Making appropriate decisions in different epidemiological and socioeconomic conditions
- Infectious diseases of animals in sub-Saharan Africa: The wildlife⁄livestock interface
- Vaccination: An approach to the control of infectious diseases
- African animal trypanosomoses
- Dourine
- Trichomonosis
- Amoebic infections
- GENERAL INTRODUCTION: COCCIDIA
- Coccidiosis
- Cryptosporidiosis
- Toxoplasmosis
- Besnoitiosis
- Sarcocystosis
- Balantidiosis
- Leishmaniosis
- Neosporosis
- Equine protozoal myeloencephalitis
- GENERAL INTRODUCTION: BABESIOSES
- Bovine babesiosis
- Equine piroplasmosis
- Porcine babesiosis
- Ovine babesiosis
- GENERAL INTRODUCTION: THEILERIOSES OF CATTLE
- East Coast fever
- Corridor disease
- Zimbabwe theileriosis
- Turning sickness
- Theileria taurotragi infection
- Theileria mutans infection
- Theileria annulata theileriosis
- Theileriosis of sheep and goats
- Theileria buffeli⁄orientalis infection
- Non-pathogenic Theileria species in cattle
- GENERAL INTRODUCTION: RICKETTSIAL, CHLAMYDIAL AND HAEMOTROPIC MYCOPLASMAL DISEASES
- Heartwater
- Lesser known rickettsial infections in animals and humans
- Chlamydiosis
- Q fever
- Eperythrozoonosis
- Bovine Haemobartonellosis
- Potomac horse fever
- GENERAL INTRODUCTION: ANAPLASMOSES
- Bovine anaplasmosis
- Ovine and caprine anaplasmosis
Lesser known rickettsial infections in animals and humans
This content is distributed under the following licence: Attribution-NonCommercial CC BY-NC  View Creative Commons Licence details here
View Creative Commons Licence details here
NJ Maclachlan and M-L Penrith (Editors). AL Fedrow, KE Mullins, ML Lehman and RL Stewart, Lesser known rickettsial infections in animals and humans, 2019.
Lesser known rickettsial infections in animals and humans
Previous authors: K J SUMPTION AND G R SCOTT
Current authors:
A L FEDROW - Assistant Professor, MS, PhD, Shippensburg University, 1871 Old Main Drive, Shippensburg, Pennsylvania, 17257, United States of America
K E MULLINS - Associate Director of Chemistry, Point of Care, and Clinical Laboratory Support, PhD, 111 Michigan Avenue, N.W., Washington DC, 20010, United States of America
M L LEHMAN - Professor, PhD, Biology Department, Shippensburg University, 1871 Old Main Drive, Shippensburg, Pennsylvania, 17257, United States of America
R L STEWART - Shippensburg University, 1871 Old Main Drive, Shippensburg, Pennsylvania, 17257, United States of America
General introduction
In 2001, the order Rickettsiales was subjected to a taxonomic reorganization based upon genetic analyses of 16S rRNA, groESL, and surface protein genes87 The major changes were in the families Rickettsiaceaeand Anaplasmataceae, including:
- the family Rickettsiaeceaewas amended to include the genera Rickettsia and Orientia; and
- the family Anaplasmataceaewas broadened to include all species in the genera Ehrlichia, Anaplasma, Cowdria, Wolbachia, and Neorickettsia. As such, the genus Anaplasma was modified: 1) to include the organisms originally designated as Ehrlichia phagocytophila, Ehrlichia bovis, and Ehrlichia platys; 2) to include Ehrlichia equi and the Ehrlichia HGE agent as synonymous with Anaplasma phagocytophilum; and 3) to place Cowdria ruminantium into the genus Ehrlichia (i.e. Ehrlichia ruminantium).87 Consequently, the re-classification resulted in nomenclature changes of certain animal pathogens that are discussed in this chapter (Table 1).
Table 1 Nomenclature changes associated with reorganization of the order Rickettsiales in 200187
| Nomenclature pre-2001 | Nomenclature after 2001 | Associated animal disease |
|---|---|---|
| Ehrlichia equi, Ehrlichia phagocytophila, Ehrlichia HGE agent | Anaplasma phagocytophilum | Tick borne fever or Pasture fever, Equine granulocytic anaplasmosis , Canine/Feline anaplasmosis |
| Ehrlichia bovis | Anaplasma bovis | Bovine anaplasmosis |
| Ehrlichia platys | Anaplasma platys | Canine cyclic thrombocytopenia |
Infections of domestic animals associated with members of the Rickettsiales were reported in Europe since approximately 1780, with historical reports describing febrile diseases (sometimes lethal) associated with tick infestations in farm animals and dogs.110, 111, 259 Members of the Rickettsiaceaeand the Anaplasmataceae are transmitted to humans by ticks, mites, fleas, and lice, and can result in disease(s) ranging from subclinical, mild, to severe to deadly. These include, Rickettsia prowazekii (the causative agent of endemic typhus), Rickettsia conorii (the causative agent of Mediterranean spotted fever), Ehrlichia chaffeensis (the causative agent of human monocytic ehrlichiosis), and A. phagocytophilum (the causative agent of human granulocytic anaplasmosis) The members of Rickettsiales that cause disease in both domestic animals and humans are not always mutually exclusive, occur worldwide, are often transmitted by specific vectors (e.g. ticks, fleas) in certain geographic regions, and vaccines are most often not available for the disease-causing agents. Despite the advent of more advanced molecular and serological diagnostic techniques, cross- reactivity among the different genera/species within the order Rickettsiales still pose a problem in making a definitive diagnosis, particularly in resource-restricted countries or laboratories.
In Africa, tick-borne pathogens are responsible for many important and serious diseases93, 226, 227, 232 resulting in livestock productivity and economic losses and may also pose public health risks. The ecological richness of the continent of Africa provides a variety of ecosystems that are ideal for supporting an array of tick/ectoparasite species, and consequently the maintenance of pathogen diversity. Moreover, close interfaces between humans and livestock/wildlife on the continent has a bearing on farming systems as well as ecotourism/tourism industries. At these interfaces there is often increased transmission of pathogens between livestock and wildlife species, resulting in the emergence of unknown pathogens or new diseases or endemicity (see Infectious diseases of animals in sub-Saharan Africa: The wildlife/livestock interface). Consequently, the need for continued and new molecular and serological surveys throughout Africa cannot be overemphasised. In this chapter, the lesser known members of Rickettsiales (Anaplasmataceae and Rickettsiaceae) are discussed, some of which have a history of causing disease amongst animals and humans in Africa.
Order Rickettsiales
Members of the order Rickettsiales are all Gram-negative, obligate intracellular bacteria vectored by either arthropods or trematodes; within their host cell they replicate in vacuoles in the cytoplasm and/or can be found within the host nucleus.224, 241 Bacteria in the order Rickettsiales that are responsible for diseases in humans and animals are associated with the genera Rickettsia (rickettsioses), Orientia (scrub typhus), Anaplasma (anaplasmoses) and Ehrlichia (ehrlichioses).
Family Anaplasmataceae (genera Anaplasma and Ehrlichia)
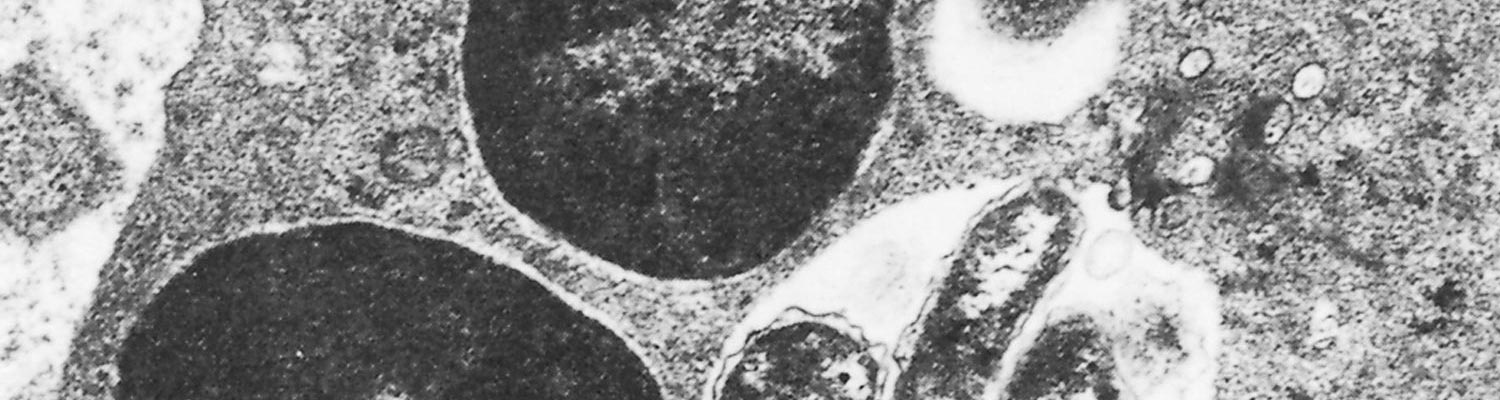
The Anaplasma and Ehrlichia are coccoid/ellipsoidal (can also be pleomorphic), multiply in membrane-bound, cytoplasmic vacuoles within their host cell forming morulae, and can be present in both reticulate and dense core forms.234, 279, 293
Anaplasma species cause disease in animals (domestic ruminants, equines, canines, felines, deer, rodents) and humans. Moreover, there have been recent reports of human infections caused by species previously thought only to infect domestic animals.20, 51, 187
Ehrlichia species infect domestic ruminants, canines, rodents, and humans.245 Ticks are the primary vectors of Anaplasma and Ehrlichia species. However, Anaplasma species can also be transmitted by biting flies, contaminated fomites, and/or via blood transfusions.22, 166, 277 The host target cells of Anaplasma and Ehrlichia are species-dependent, with a predominance of infection occuring in erythrocytes, monocytes, macrophages, granulocytes, endothelial cells, and/or platelets.279, 293 As observed throughout the order Rickettsiales, symptoms associated with Anaplasma and Ehrlichia infections are often flu-like, and can be mild or progress to severe/lethal outcomes; the course of disease in animals and humans is dependent upon the infecting strain. The tetracyclines (doxycycline) are the antibiotic of choice for treatment of Anaplasma and Ehrlichia speciesinfections;120, 316 some fluoroquinolones are effective against some Anaplasma species,196 and chloramphenicol has been described with both failure and success in the treatment of Ehrlichia infections.27, 95, 115, 186
Some Anaplasma and Ehrlichia species that cause livestock disease are well known in Africa, particularly those species associated with bovine and ovine and caprine anaplasmosis (Anaplasma marginale, Anaplasma ovis, and Anaplasma centrale), and heartwater/cowdriosis (Ehrlichia ruminantium). Molecular and serological surveys have revealed the presence of Anaplasma and Ehrlichia species in animals, humans and/or ticks previously not known to harbour them, Moreover, newly identified/unclassified Anaplasma and Ehrlichia species, with proposed zoonotic potential, have been reported recently in Africa. In this chapter, the lesser known species associated with infections in Africa are dealt with, including Anaplasma bovis, Anaplasma platys, Anaplasma phagocytophilum, Ehrlichia chaffeensis, Ehrlichia canis, Ehrlichia ewingii, and Ehrlichia muris.
Rickettsia species infections
The Rickettsia bacteria are short rods (paired in some instances), 0.3-0.5 x 0.8-2.0 µm, free in the cytoplasm of host cells, or in some instances intranuclear, and divide by binary fission.293 Within the genus Rickettsia, the species are divided into the spotted fever group rickettsiae, the typhus group rickettsiae, and the ancestral/transitional group.202 Hard ticks (Ixodidae) are the primary vectors of the spotted fever group rickettsiae in hosts such as humans, livestock, canines, felines, birds, and reptiles. Some members of the spotted fever group rickettsiae maintainance vector hosts are fleas (R. felis48 and R. asembonensis),189 tsetse flies, mites, mosquitoes, ticks (R. felis-like organisms (RFLO)),218 soft ticks in the Argasidae family (R. hoogstraalii85and Candidatus R. lussitaniae) and mouse mite (Liponyssoides sanguineus)127 (R. akari). Fleas and lice are the vectors of the typhus group rickettsiae, which are transmitted to humans upon contamination of the vector bite site with the faeces from the infected vector.13
Following the bite of an infected host, rickettsiae disseminate via the bloodstream and replicate in the cytoplasm primarily of endothelial cells.244 Flu–like symptoms are usually associated with rickettsial infections in humans, and an eschar may be present at the site of the vector bite. Disease can range from mild to lethal.224 Doxycycline is the drug of choice for treatment of diseases associated with species of the Rickettsia genus but other tetracyclines, chloramphenicol, rifampin, fluoroquinolones, and some macrolides have also been used.47, 239
The potential for bacteria of the genus Rickettsia to cause disease in domestic animals in Africa has only recently become clearer, primarily due to the availability of advanced molecular techniques to identify and characterize these agents. Most studies in Africa in livestock focused on the presence of the rickettsial agent(s) in ticks collected from the host and/or the immediate surroundings and serological evidence of infection in their hosts. Despite the paucity of information about the pathogenicity of Rickettsia species in livestock, it is important to consider their disease-causing and zoonotic potential in the diverse ecological or climatic niches at the human/animals interfaces in Africa.
Anaplasma bovis infections (Bovine anaplasmosis; Monocytic anaplasmosis)
Anaplasma bovis is one of the causative agents of bovine anaplasmosis or monocytic anaplasmosis (formerly bovine ehrlichiosis)83, 87, 245, 259 in Asia and Africa.245, 259 Early reports of the disease implicated A. phagocytophilum, an organism capable of infecting granulocytes, as the disease causative agent.118, 130, 245, 259
Anaplasma bovis primarily infects circulating monocytes,39, 87, 174, 292 but may also infect tissue macrophages.317 It has been reported in ruminant species (cattle, goats and wild deer),57, 174, 317, 319 small wild animals,194 dogs,262 cats,270 and rabbits.108 It has been suggested that small mammals are reservoirs of A.bovis.108, 259
Anaplasma bovis are small pleomorphic coccoid to ellipsoid cells, approximately 0.3 µm in diameter, with a similar morphology to other members of the genus.293 It has not yet been cultivated in vitro,87, 293 but can be propagated by serial passage in cattle.293 The parasites in bovine monocytes stain dark blue with Romanowsky methods.87, 293 Although the host cell ligand is not known for this species, another member of the group, A. phagocytophilum, utilizes the platelet glycoprotein selectin ligand 1 (PGSL-1) to bind to host cells.87, 121 The organism is internalized and remains within vacuoles in the infected cell in vivo.293
Phylogenetic analysis demonstrated that A. bovis was more closely related to A. phagocytophilum than to either A. marginale or A. centrale.87 A more recent study in 2014 showed that it consistently fell into the cluster that included A. phagocytophilum, A. platys and Anaplasma sp. Japan.34, 321 Studies of the genetic variability of A. bovis recovered from different geographic regions and different hosts demonstrated that similarity between strains exceeds 99 per cent.139, 141, 245, 271
There are few studies on the prevalence of A. bovis infections. Anaplasma bovis has been reported in countries in Africa, North America, Japan and Brazil,108, 141, 267 although most reports of infection in ruminants emanated from African countries. In Tunisia and Algeria in North Africa259 A.bovis has been reported in cattle, sheep and goats, but not in camels.29-32, 38, 255 Tunisian cattle had a prevalence rate of 3.9 per cent for A.bovis,25.4 per cent for A. marginale and 15.1 per cent for A. centrale.29 Another study showed prevalence rates of A. bovis in South Mediterranean sheep and goats of 42.7 and 23.8 per cent, respectively.38 This study demonstrated that the strains of A. bovis isolated from goats and sheep clustered with other strain sequences previously published in GenBank and were similar to the results from sequence analysis conducted in Tunisian cattle.29 It was suggested that sheep and goat populations could play a key role in the bovine anaplasmosis disease cycle in the Mediterranean region of Tunisia.34 A more recent study in the north of Tunisia that utilized molecular techniques showed an overall prevalence rate of 4.9 per cent for A. bovis infection in cattle.31 A separate longitudinal field study in Mediterranean sheep and goats demonstrated the average prevalence of A. bovis was 7.4 per cent in sheep and 10.1 per cent in goats.30 The infection rates in cattle and sheep varied seasonally.30, 31 The A. bovis prevalence rates in these studies were lower than those of an earlier Tunisian study (sheep 42.7 per cent and goats 23.8 per cent),38 as well as rates in other ruminant populations from different geographic regions, including goats in China (49.6 per cent) and deer (23 per cent) and cattle (15-53.3 per cent) in Japan.135, 141, 174 These rates were higher than reported in cattle populations from Iran, India and Italy (2.7 per cent, 3.3 per cent and 4.2 per cent, respectively).57, 210, 215 Various factors were incriminated as an explanation for these different prevalence rates.30, 38
In a study conducted in northeast Algeria, A. bovis infection was demonstrated to be 4.4 per cent in cattle,255 similar to the rate observed in a Tunisian study.31 The A. bovis variant detected in cattle in the recent Algerian study demonstrated high homology with other A. bovis variants isolated from cattle, goats and sheep in Tunisia,29, 31, 39 variants isolated from Haemophysalis longicornis ticks in South Korea and variants isolated from wild deer populations in Japan.255 The authors indicated that this was the first report demonstrating the presence of A. bovis (along with other Anaplasma spp.) in cattle in this region.
Anaplasma bovis infections are usually subclinical but clinical signs may include fever, weight loss, weakness, anaemia, depression, enlarged lymph nodes, and pale mucous membranes.29, 39, 215, 267, 306 Abortion and death occur rarely.39, 259, 267 Treatment with tetracyclines can be used in severe cases of A. bovis.
Multiple tick vectors have been implicated in the transmission of A. bovis. In Africa Amblyomma variegatum and Rhipicephalus appendiculatus have been implicated but different vectors, such as a Hyalomma sp. in Iran and Amblyomma cajennense in Brazil are also considered to be vectors.87, 245, 307 Anaplasma bovis or A. bovis-like organisms have been detected in different Haemaphysalis spp. including H. longicornis in Korea and Japan,141, 151 Haemaphysalis concinna in Russia,255 Haemaphysalis lagrangei in Thailand264 and Dermacentor andersoni in Canada.78
Anaplasma platys infections (Infectious canine cyclic thrombocytopenia (ICCT))
Anaplasma platys (formerly known as Ehrlichia platys)is the causative agent of infectious cyclic thrombocytopenia (ICCT) in dogs, infecting platelets. It occurs worldwide.89, 259 The bacterium was first identified in dogs from Florida, United States of America(US).118 It is assumed to be vectored by Rhipicephalus sanguineus senso lato (brown dog tick), although the tick’s competence as a vector has not been definitively established.280 Anaplasma platys has also been detected in Ixodes ricinus, Ixodes persculatus, Hyalomma detritum, Hyalomma excavatum, Haemaphysalis longicornis, Rhipicephalus camicasi, Rhipicephalus evertsi, Rhipicephalus pulchellus, and Rhipicephalus pravus,suggesting that the bacterium may be vectored by a variety of ticks.152, 195, 221, 269
In dogs, ICCT is characterized by thrombocytopenia, fever, weakness, lethargy, anorexia, ocular discharges, splenomegaly, hyperkeratosis of the muzzle, and respiratory signs.260 The incubation period of A. platys is one to two weeks, which is followed by cyclical periods (every one totwo weeks) of thrombocytopenia and fever.104 The severity of the clinical signs14, 18, 68, 288 is influenced by the breed, age and immune status of the dog: fatalities are uncommon unless fatal haemorrhaging occurs following accidents or surgery.245 While the disease is often asymptomatic/subclinical in the US and Australia, it is clinically more severe in South America, Europe, Africa, and Asia.49 This discrepancy is possibly due to co-infections with other pathogens, but is more likely the result of A. platys strains and/or A. platys-like strains with different pathogenicity.49 Infections are commonly treated with tetracyclines (particularly doxycycline) for 8-10 days or with enrofloxacin for 14-21 days.261
Anaplasma platys has not yet been cultivated in vitro and no vaccine against A. platys is available.
In addition to infecting dogs, Anaplasma platys has a wide host range and may also infect sheep, goats, cattle, dromedary camels, buffalo, and deer,8, 32, 35, 40, 61, 67, 81, 163, 177, 178, 184 as well as humans20, 51, 187 and cats.172, 263 Anaplasma platys infections have been reported in dogs and/or ticks collected from dogs64, 112, 162, 191, 195, 265, 269, 275 throughout Africa. Apart from fever, most infections in the abovementioned animal species are subclinical.
Anaplasma phagocytophilum infections (Tick-borne fever or Pasture fever)
Anaplasma phagocytophilum is the causative agent of tick-borne fever (TBF) or pasture fever in domestic ruminants (primarily sheep and cattle), and human granulocytic anaplasmosis (HGA) and also infect dogs, cats, goats, donkeys, horses, and deer. Cattle, sheep, wild ruminants (cervids), and rodents (white-footed mouse) are thought to serve as reservoirs of A. phagocytophilum, although definitive reservoir hosts have not yet been identified.21
In Europe, A. phagocytophilum has long been a well-known agent of disease in domestic ruminants, where it was first described as a “Rickettsia” in sheep during the early 1900s.110, 111 The bacterium was first associated with human infection in 1994 in the US, and was originally referred to as the “human granulocytic ehrlichia agent”.59 Anaplasma phagocytophilum primarily infects neutrophils in cattle, sheep, goats, horses, deer, dogs, and humans99, 100, 299 Morulae can be observed in infected cells. In both animals and humans, disease can range from subclinical or mild to severe and can be fatal The severity of infection is dependent upon a multitude of factors, including, age, immune status of the host, host species, and the variant of A. phagocytophilum that is causing the infection. Infections in domestic ruminants are often characterized by high fever, anorexia, lethargy, weight loss, reduction in milk production, and abortion.102, 113, 259, 296, 299 Similar signs are observed in other susceptible animal species. In addition, petechial haemorrhages in horses,99 depression and lameness in dogs,88 and hyperaesthesia, conjunctivitis, and incoordination in cats have been associated with the disease.45, 119 In humans, symptoms associated with HGA manifest one to two weeks after the bite of an infected tick and are generally flu-like, including fever, headache, myalgia, and lethargy. Thrombocytopenia, leukopenia, and liver damage have also been reported.25, 310 In the US, the case fatality rate associated with A. phagocytophilum infections is less than 1 per cent,41 and hospitalization rates have been reported at 36 per cent, of which 7 per cent of the patients needed intensive care.86 Human infections are much less frequently reported in Europe and Asia. However, serosurveys revealed antibodies in humans throughout both continents.245 The drug of choice for treatment of human infections is doxycycline (rifampicin can be used as an alternative if necessary).24 In domestic animals, prophylactic treatment with tetracycline has been used when moving animals into tick infested pastures.52 Long-acting oxytetracycline is effective in treating infections in domestic ruminants, horses, dogs, and cats.21
Anaplasma phagocytophilum has been detected by molecular methods in a variety of tick species, but the vector competence has only been demonstrated for Ixodes scapularis, Ixodes pacificus, Ixodes ricinus, and Ixodes spinipalpis.315 In North America, A. phagocytophilum has been detected in I. pacificus, I. spinipalpis, Dermacentor variabilis, and Dermacentor occidentalis in the western parts of the USA;124, 161, 324 I. scapularis and Amblyomma americanum in the eastern, upper midwestern and southern USA63, 179, 256 and I. scapularis and Dermacentor albipictus in Canada.26, 158 Similarly, A. phagocytophilum has been detected in a wide range of tick species throughout Europe including I. ricinus (the main vector), Ixodes persulcatus, Dermacentor reticulatus, Haemaphysalis concinna,and Ixodes ventalloi.231, 266, 297, 303 In Africa, although fewer surveillance studies for A. phagocytophilum have been performed compared to other tick-borne diseases, the studies have nonetheless revealed the molecular presence of the bacterium in multiple species of ticks including Rhipicephalus sanguineus (Egypt);105 Amblyomma variegatum, Amblyomma lepidum, Amblyomma cohaerens (Ethiopia);125, 301 Hyalomma marginatum, Hyalomma excavatum, Rhipicephalus bursa, I. ricinus, R. sanguineus, Hyalomma detritum (Algeria, Tunisia, Morocco);183, 269 Rhipicephalus evertsi evertsi, Rhipicephalus decoloratus, Amblyomma hebraeum (South Africa);207 Rhipicephalus pulchellus (Kenya);223 and Amblyomma flavomaculatum (collected from lizards imported from Ghana).217 The abovementioned ticks were collected from animals (domestic or wild), and from vegetation of a wide range of habitats.
The occurrence of A. phagocytohilum (and its variants) in domestic and wild animals and humans has been reported in a limited number of studies in Africa including in humans in Morocco,148 and dogs in Tunisia, Morocco, Algeria, South Africa, and Cape Verde.23, 147, 153, 157, 182 In Tunisia, immunofluorescence assays (IFA) and nested polymerase chain reaction (PCR) assays and DNA sequencing were used to detect the presence of A. phagocytophilum in healthy horses.37, 183
In Europe, A. phagocytophilum has been reported to cause persistent infections in sheep that may act as a reservoir.295 Anaplasma phagocytophilum has been identified in the blood of clinically ill sheep in Senegal using PCR and DNA sequencing.81 In Algeria, infected dairy cows showed fever, decreased milk production, cough, and oedema of the distal parts of the body.67 The widespread occurrence of infection in Africain a variety of both ticks and mammals underscores the need for additional surveillance and transmission studies.
Variants based on the highly conserved 16S rRNA gene56 of A. phagocytophilum have been detected in ticks and domestic/wild animals worldwide. Among the 15 genetic variants that have been recognized based on comparison of the 5’ variable fragments of the 16S rRNA gene, variants 1 (accession number U02521, prototype strain, Ap-ha) and 2 (accession number AF093789, CAHU-HGE1) are most often reported in surveillance studies.245 Variants 1 and 2 have been reported in I. scapularis, I. ricinus, I. persulcatus, and Ixodes ovatus ticks, as well as in sheep, cattle, horses, dogs, cats, deer, and bison in both the US and Europe.59, 193, 298, 309 Moreover, human cases of anaplasmosis associated with both variants have been reported in the US.58, 59 In Africa, closely related variant strains of A. phagocytophilum have been reported in sheep, goats, and cattle from Tunisia and Algeria and have also been detected in ticks and mammals in Japan and China.34, 36, 67, 135, 139, 220, 320, 323
Ehrlichia chaffeensis infections (Canine ehrlichosis, Human monocytic ehrlichiosis)
Ehrlichia chaffeensis is a causative agent of both human monocytic ehrlichiosis and canine ehrlichiosis in North America, South America, Asia, and Africa. It is transmitted by ticks245 and infects monocytes and macrophages. Amblyomma americanum was the first tick species identified as a vector for E. chaffeensis in the US, in 1993.12, 72, 74 Since then, E. chaffeensis has been detected in a variety of tick species including Ixodes pacificus and Dermacentor variabilis in the US, Haemaphysalis longicornis and Ixodes persulcatus in South Korea, Dermacentor silvarum, Amblyomma testudinarium and Haemaphysalis yeni in China, Amblyomma parvum in Argentina,55, 151, 165, 272, 304, 312 Hyalomma impeltatum in Nigeria and in Rhipicephalus sanguineus in Cameroon.212, 252
Ehrlichia chaffeensis was first isolated in1991 from a patient with symptoms of human monocytic ehrlichiosis.10, 212, 245 Human monocytic ehrlichiosis was first described in 1987 and thought to be caused by E. canis, but it is possible that E. chaffeensis was the aetiologic agent in this case.12, 186, 212, 245 While, E. chaffeensis DNA has been detected in febrile patients in Cameroon, the organism has only been isolated from symptomatic humans in the US.245, 247 Various Ehrlichia species (E. canis, E. ewingii, E. chaffeensis ) may cause canine ehrlichiosis.73, 245
There is a close relationship between E. chaffeensis and E. canis. and both can infect dogs.50, 71, 73, 170, 173 Dogs infected with E. chaffeensis may show fever, lethargy and thrombocytopenia.50, 170, 173 Experimental infection of dogs showed that E. chaffeensis can result in persistent infections lasting at least two to four months, thereby providing evidence that dogs are likely a reservoir for E. chaffeensis.328 North American white-tailed deer can become infected with E. chaffeensis and are believed to be reservoirs of the parasite.71, 72, 173, 245 Erlichia chaffeensis has been detected in many vertebrate hosts including goats in China and the US, Sika deer in Japan and South Korea, coyotes in the US, and wild rats in China.84, 156, 164, 312, 327
In an attempt to better understand E. chaffeensis, red and grey foxes, white- tailed deer, and calves were experimentally infected with E. chaffeensis,69, 74, 77, 308which resulted in persistent infections in white-tailed deer70, 74, 308 and red but not grey foxes,69 Calves developed mild clinical signs such as fever, neutropenia, and thrombocytopenia to severe disease with lethargy, muscular weakness, and death.77 Amblyomma americanum and Dermacentor variabilis ticks that fed on the infected calves became infected with E. chaffeensis.77
Ehrlichia canis infection (Canine monocytic ehrlichiosis)
Ehrlichia canis was first described in dogs from Algeria in 1935.82 It occurs worldwide causing canine monocytic ehrlichiosis and ehrlichiosis in humans, with increased infection rates in tropical and subtropical regions.82, 245, 281 The main vectors are Rhipicephalus sanguineus and Dermacentor variabilis82, 97, 114, 136, 213, 233, 245, 281but E. canis has also been recovered from Haemaphysalis sulcata and Dermacentor marginatus in Italy and from Haemaphysalis longicornis and Ixodes turdus in South Korea,152, 272 and Rhipicephalus bursa in Sardinia. Few studies have been undertaken to determine if livestock are susceptible to infection with E. canis.192
Dogs and wild canids such as silver backed jackals, coyotes, red and grey foxes, and wolves and wolf x dog hybrids, are reservoir hosts for E. canis.82, 97, 114, 236, 245, 299 Rhipicephalus sanguineus and Dermacentor variabilis ticks have been shown experimentally to acquire infections from dogs and were able to transmit E. canis to dogs.82, 97, 114, 136, 236
Subclinical infections are common in dogs. Canine monocytic ehrlichiosis can result in subclinical infection and acute and chronic disease.65, 245, 254 Canine ehrlichiosis caused by E. canis is much more severe than disease caused by other Ehrlichia species.65, 245, 254 Acute disease is characterized by an incubation period of 8-20 days, fever, depression, dyspnoea, anorexia, splenomegaly, thrombocytopenia, leukopenia, anaemia, and hypergammaglogulinaemia and the presence of parasites in monocytes.65, 117, 245, 281 Subclinical infections can last for years in otherwise healthy dogs. Chronic canine monocytic ehrichiosis is usually the most severe form of the disease, leading to lethargy, anorexia, weight loss and death.117, 281
A novel Ehrlichia most closely related to E. canis has been detected in North American and Brazilian cattle, and a calf experimentally infected with it exhibited clinical signs of ehrlichiosis including fever, depression, lethargy, and thrombocytopenia.4, 101
Ehrlichia ewingii infections (Canine granulocytic ehrlichiosis)
Ehrlichia ewingii, unlike other Ehrlichia species, infects granulocytes, and was first identified as a new strain of E. canis causing canine granulocytic ehrlichiosis in 1971, but was later realized to be a completely different species of Ehrlichia, and subsequently named E. ewingii in 1992.10, 245, 318 Ehrlichia. ewingii occurs in the US, Africa, and Asia. It is the cause of human ewingii ehrlichiosis.11, 54, 245 Amblyomma americanum and Dermacentor variabilis in the US, Rhipicephalus sanguineus in the US and Cameroon, and Haemaphysalis longicornis in Korea have been shown to harbour E. ewingii.19, 152, 209, 213, 294 Amblyomma. americanum has been shown experimentally to transmit E. ewingii to dogs.19
Ehrlichia ewingii causes a much milder disease in dogs than E.canis65, 109, 170, 245, 318and clinical signs include fever, lameness, neutrophilic polyarthritis, and thrombocytopenia.11, 19, 65, 109, 245 Most E. ewingii infections in dogs are subclinical, leading to the belief that dogs are a reservoir host for E. ewingii.1, 2, 13, 50 Like E. chaffeensis, white-tailed deer in the US seem to be a reservoir host for E. ewingii.245, 318
Recently, E. ewingii has been suggested as a possible cause of a febrile illness in goats in the US, after E. ewingii-infected A. americanum ticks were fed on them.175 These goats showed fever, nasal discharge, lethargy, and neutropenia and became chronically infected and were able to transmit E. ewingii to A. americanum ticks.175
Ehrlichia muris infections (Murine splenomegaly)
Like E. canis and E. chaffeensis, E. muris infects monocytes and macrophages. Its distribution is currently limited to Eurasia.245 Vectors for E. muris are Haemaphysalis species and Ixodes species including Haemaphysalis flava in Japan, Ixodes ricinus in Europe, and Ixodes persulcatus in Russia and Japan.7, 92, 128, 140, 159, 186, 245, 246, 248, 278, 289 Small rodents are the reservoir host for E. muris, as it has been detected in voles, field mice, shrews, and Siberian chipmunks in Russia, yellow-necked mice in Slovakia, and wild mice in Japan.140, 245, 246, 289 Mice have been shown to exhibit moderate splenomegaly due to infection with E. muris.313 Sika deer in Japan have been found to harbour E. muris.300 Antibodies to E.muris have been detected in dogs, mice, monkeys, bears, and deer in Japan.140
Genus Rickettsia
Diseases associated with the genus Rickettsia have a long, extensive history of plaguing mankind – both military and civilian populations;142 currently several rickettsial pathogens are considered to be emerging infectious agents and are noted as public health issues.227 Rickettsial pathogens can be found throughout the world, primarily as a result of the cosmopolitan nature of their associated vectors (ticks, fleas, lice, and mites). Currently, there are more than 25 recognized rickettsial species in the spotted fever group and two species in the typhus group.60 As observed with the organisms of the Anaplasmataceae, rickettsial pathogens and their associated vectors occur frequently at human/animal interfaces, underscoring the need for continued surveillance these often-emerging infectious agents. Here, we discuss those Rickettsia that have been detected in surveillance studies, in Africa, many of which have also been detected in several tick species and countries all over the world, (see Table 2).5, 44, 75, 98, 106, 116, 149, 154, 169, 203, 222, 227, 228, 235, 237, 238, 243, 274, 290, 302, 326
Rickettsia felis infections
Rickettsia felis was first identified in Ctenocephalides felis (commonly known as the cat flea) in the US in 1990.3 It is recognized as the causative agent of flea-borne spotted fever (aka cat-flea typhus, R. felis rickettsiosis). Fleas, ticks, mites, lice, and mosquitoes are potential vectors of R. felis.1, 80, 250, 286 Despite the detection of R. felis in a many potential vectors, the cat flea (Ctenocephalides felis) is currently the only recognized vector of R. felis.
Rickettsia felis infections in humans have been reported in countries in North America, South America, Europe, Africa, Asia, and New Zealand and Australia.171, 251, 314 Infection and disease associated with R. felis is widespread in Africa.89 In Senegal, Kenya, Mali, Tunisia, and Algeria, 1-5 per cent of human febrile diseases were shown to be linked to infection with R. felis.201, 253, 285 However, other studies have reported R. felis infections associated with febrile diseases to be as high as 10-15 per cent in Senegal and Gabon.201, 206 Rickettsia felis has been detected in the blood and/or in fleas collected from domestic and wild animals, including dogs, cats, rodents, hedgehogs, and monkeys on several continents.6, 122, 123, 167, 257
Recent studies detected R. felis-like organisms (RFLOs) in in a variety of ectoparasites. Among the RFLOs are Rickettsia asembonensis (fleas from Kenya180, 189), Rickettsia species F144 and F143 (fleas from Thailand96), Rickettsia species SE313 (fleas and mites from rats in Egypt176), Rickettsia species RF2125 (fleas from the Thai-Myanmar border,229 US,214, 249 and Hungary,126), Rickettsia species clone ric_Ag_101731 (mosquitoes from the Ivory Coast286), and Rickettsia species SG10 (tsetse flies in Senegal198). Full characterization studies including isolation in pure culture of these RFLOs are needed in order to better define their importance and pathogenicity in mammalian hosts.
Rickettsia typhi infections
Rickettsia typhi is the causative agent of flea-borne (endemic) typhus, and is vectored by the Oriental rat flea (Xenopsylla cheopis), with rodents (primarily Rattus rattus and Rattus norvegicus) serving as the reservoir hosts of the bacterium. Besides the rat flea, R. typhi has been detected in other flea species including Xenopsylla brasiliensis (Tanzania),168 Ctenocephalides felis (Spain),216 Leptopsylla segnis (Cyprus),62 Ctenophthalmus congeneroides and Rhadinopsylla insolita (Korea).155 Moreover, R. typhi has also been detected in ticks, lice, and mites,107, 110 indicating the possibility of a wide variety of vectors in the transmission of R. typhi. Rickettsia typhi has been detected in various rat and mouse species, shrews, opossums, and cats,46, 160, 216 as well as in domestic ruminants in Egypt.273Murine typhus was recognized as a different disease from epidemic typhus (Rickettsia prowazekii) in the 1920s.197 199 It has a worldwide distribution in a variety of climates, and is often found in port or coastal cities where rodents can be commonly found.142 In Africa, there are few studies on the prevalence of R. typhi. It has been detected in fleas collected in Algeria, Benin, and Tanzania.43, 168 Human disease associated with murine typhus in Africa has been reported from Algeria, Tunisia, Morocco, Ivory Coast, Central African Republic, Madagascar, Reunion, Chad, Tanzania, and Senegal.15, 17, 103, 204, 311, 329 It has been suggested that the disease in Africa is possibly under reported considering the wide distribution of its vectors and reservoirhosts.
Rickettsia africae infections
Rickettsia africae is the causative agent of African tick bite fever (ATBF) and is known to be the most prevalent tick-borne rickettsiosis in sub-Saharan Africa.190 It is often found to be the cause of illness in tourists visiting countries in sub-Saharan Africa.9, 131, 133, 242 The ticks that are recognized as the principle reservoir hosts or vectors of R. africae are Amblyomma hebraeum and Amblyomma variegatum132 (see Tick vectors: an African perspective). It has been demonstrated that these ticks can maintain infection with R. africae both transovarially and transtadially, allowing for transmission of the bacteria to animals and humans during all of these ticks’ life cycle stages.150, 283 Infection rates of these tick species tends to be very high, with rates of almost 100 per cent in endemic areas.211, 225 In addition to A. hebraeum200, 264 and A. variegatum, R. africae has also been detected in a variety of ticks throughout Africa, although their role in the transmission of R. africae has not been determined yet. These include Amblyomma lepidum,208 Amblyomma compressum,200 Hyalomma marginatum rufipes,90 Hyalomma impeltatum,219 Hyalomma impressum,90 Haemaphysalis paraleachi,200 Rhipicephalus annulatus,199, 200, 252 Rhipicephalus evertsi evertsi,199, 252 Rhipicephalus decoloratus,200, 219 Rhipicephalus geigyi,200 Rhipicephalus sanguineus,219 and Rhipicephalus microplus.90 Rickettsia africae variants have been identified in various tick species throughout Africa (i.e. Kenya, Niger, Mali, Sudan, Burundi, Mauritania);91, 181, 225 however, it has not been determined whether or not the variants are associated with ATBF.
Rickettsia africae is closely associated with animals in Africa including cattle, sheep, goats, and wild ruminants due to the main vectors’ (A. hebraeum, A. variegatum) preference for these hosts.188 In particular, 80-100 per cent of cattle in endemic areas have been shown to have high seroreactivity to SFG rickettsiae, leading to the assumption that cattle may be involved in maintenance of the pathogen.143, 144, 230 Similarly, high seroprevalences have also been observed in goats and sheep.143, 188, 230 Despite seroprevalence among livestock, the levels have not been shown to be exclusively linked to exposure of the animals to ticks infected with R. africae,188 emphasizing the necessity for additional studies to better understand the relationship between the vectors of R. africae, their livestock hosts, and associated human infections.
Rickettsia aeschlimannii was isolated in 1992 from Hyalomma marginatum marginatum ticks in Morocco226 and the first case of spotted fever due to infection with R. aeschlimannii was in a patient who had travelled to Morocco.240 More recently, cases have been reported in Algeria and South Africa.205, 226 Ticks of the genus Hyalomma are suspected to be the main vectors,42 and the bacterium has been detected in H. marginatum marginatum (Algeria, Morocco, Egypt),2, 44, 86 Amblyomma variegatum (Nigeria),252 Hyalomma impeltatum (Nigeria, Senegal),252, 264 Hyalomma marginatum rufipes (Mali, Niger, Senegal, Nigeria, Ivory Coast)90, 137, 225, 264Hyalomma truncatum (Senegal, (Ivory Coast),90, 199 Rhipicephalus evertsi evertsi (Nigeria, Senegal)252, 264 and Rhipicephalus annulatus (Nigeria).252 The ticks in which R. aeschlimannii was detected were collected from domestic animals such as cattle, sheep, goats, donkeys, horses, and camels; however, no link between infections in animals and humans has yet been demonstrated.
Rickettsia conorii infections
Rickettsia conorii subsp. conorii is the causative agent of Mediterranean spotted fever (MSF) in humans and is vectored by Rhipicephalus sanguineus ticks. The disease was first reported in humans in 1910 in Tunisia.66 More recent cases of MSF have been reported in Algeria, Tunisia and Morocco,146, 258 as well as among travellers returning from Senegal and other countries in sub-Saharan Africa.33, 53, 199, 322 The animal reservoir associated with R. conorii subsp. conorii has not been explicitly defined; however, dogs and hedgehogs have been suggested, based on seroprevalence studies and human proximity to dogs as risk factors for contracting MSF.44, 232, 287 Additionally, R. conorii has been detected in ticks (Rhipicephalus mushamae, Haemaphysalis leachi, Rhipicephalus simus, Rhipicephalus evertsi evertsi, Haemaphysalis punctaleach) removed from domestic animals (cattle, dogs, and/or horses) in the Central African Republic, Zimbabwe, Senegal, and Uganda.199, 226, 284 The role of these ticks as vectors of R. conorii has not yet been determined.
Rickettsia conorii subsp. israelensis is also vectored and maintained transstadially325 by Rhipicephalus sanguineus. It is the causative agent of Israeli spotted fever (ISF) in humans, and dogs have been implicated as reservoir of the bacterium.28, 305 The cases of ISF reported in Tunisia were in patients who did not report tick bites, but were in close association with dogs and/or worked in the livestock industry.321 The bacterium has been detected in R. sanguineus ticks and in the blood of a dog in Nigeria.138
Rickettsia massiliae infections
Rickettsia massiliae was first isolated from Rhipicephalus sanguineus ticks in 1992 near Marseille, France.227 It has been reported as a human pathogen in Europe and South America; in Africa reports of human infection are scant. One study in Tunisia reported the presence of R. massiliae DNA in a patient.150 The bacterium has been detected in many species of Rhipicephalus ticks in countries in North and West Africa (Algeria, Morocco, Senegal, Guinea, Nigeria, Ivory Coast).89, 227 In particular Rhipicephalus ticks collected from donkeys, cattle, and dogs showed high rates of infection, along with ticks collected from the vegetation,199, 200, 252 suggesting several possible reservoirs, as well as its subsistence in nature. Rickettsia massiliae was detected recently in the blood of cattle in Nigeria.178
Rickettsia sibirica infections
Rickettsia sibirica subsp. mongolitimonae is the causative agent of lymphangitis-associated rickettsiosis (LAR), and was first isolated in 1991 from Hyalomma asiaticum ticks collected in Mongolia.226 Cases of LAR have been reported in visitors to Algeria, Egypt, and South Africa.98, 226, 282 In Senegal, infected Hyalomma truncatum ticks have been collected from cattle, donkeys, sheep, goats, and horses.199
Rickettsia slovaca and Rickettsia raoultii infections
Both R. slovaca and R. raoultii have been linked to the syndrome scalp eschars and neck lymphadenopathy (SENLAT) following tick bites in 2010.16 The syndrome has also been termed tick-borne lymphadenopathy (TIBOLA) and/or DEBONEL (Dermacentor-borne necrotic erythema and lymphadenopathy).227 The bacteria have been detected in both Dermacentor marginatus and Dermacentor reticulatus ticks94, 134, 190 and serologically and molecularly in the blood of sheep, goats, and cattle in Europe.222, 226, 227 Dermacentor marginatus ticks collected in Morocco and Algeria have been shown to harbour the agents of SENLAT.145, 268
Rickettsia monacensis infections
Rickettsia monacensis was first identified as a human pathogen in 2005 in Spain and Italy,129, 185 and Ixodes ricinus ticks are the presumed vector.227 The bacterium has been detected in I. ricinus ticks collected in Morocco, Tunisia, and Algeria.79, 145, 268, 276
Rickettsia helvetica infections
Rickettsia helvetica is vectored by Ixodes ricinus, the natural reservoir of the bacterium.227 In Europe, R. helvetica has been isolated from blood and/or tissue samples of hedgehogs, lizards, mice, deer, and wild boar.76, 291 The bacterium has been found in I. ricinus ticks in Morocco, Tunisia, and Algeria.145, 268, 276
Table 2 Lesser known Rickettsia and their potential vectors, reservoirs, and geographical distribution
| Disease | Potential Vectors | Potential Non-Human Reservoirs | Geographical Location | |
|---|---|---|---|---|
| Rickettsia africae | African tick bite fever | Hyalomma dromedarii Hyalornma excavatum Hyalomma impeltatum Hyalomma turanicum | Camel Horse | Algeria, Ethiopia, Sudan |
| Rickettsia conorii | Astrakhan fever Boutonneuse fever Indian tick typhus Israeli spotted fever Kenyan tick typhus Mediterranean spotted fever | Rhipicephalus sanguineus | Dog Hedgehog | Algeria, Tunisia, Belgium, Bulgaria, Croatia, France, Greece, Italy, Poland, Portugal, Romania, Spain, Ukraine |
| Rickettsia aeschlimannii | Spotted fever | H. dromedarii H. turanicum H. excavatum Hyalomma detriturn | Camel Horse Sheep | Algeria, France, Germany, Hungary, Italy, Portugal, Russia, Spain, Turkey |
| Rickettsia massiliae | Spotted fever | R. sanguineus Rhipicephalus turanicus | Cattle Dogs Hedgehog | Algeria, Tunisia, France, Israel |
| Rickettsia sibirica | Lymphangitis-associated Rickettsioses (LAR) | Hyalomma anatolicum Hyalomma asiahcum H. excavatum Hyalomma truncatum H. turanicum Rhipicephalus pusillus | Camel Horse | Algeria, France, Greece, Israel, Portugal, Spain; Sub-Saharan Africa and Asia |
| Rickettsia sibirica siberica | Siberian Tick Typhus | Dermacentor nuttalli Dermacentor marginatus Dermacentor reticulatus Dermacentor silvarum Dermacentor sinicus Haemaphysalis concinna Haemaphysalis yeni Ixodes persulcatus | Unknown | Eastern China, Siberia |
| Rickettsia slovaca | Spotless Rickettsiosis | D. marginatus D. reticulatus D. silvarum | Cattle Goats Horses Sheep Wild Boar, Small mammals (Apodemes sp., Myodes glareolus) | Algeria, Morocco, France, Hungary, Italy, Russia, Slovakia, Spain, Asia |
References
- ABDAD, M., STENOS, J. & GRAVES, S., 2011. Rickettsia felis, an emerging flea-transmitted human pathogen. Emerging Health Threats Journal, 4, 7168.
- ABDEL-SHAFY, S., ALLAM, N. A., MEDIANNIKOV, O., PAROLA, P. & RAOULT, D., 2012. Molecular detection of spotted fever group rickettsiae associated with ixodid ticks in Egypt. Vector-Borne and Zoonotic Diseases, 12, 346-359.
- ADAMS, J. R., SCHMIDTMANN, E. T. & AZAD, A. F., 1990. Infection of colonized cat fleas, Ctenocephalides felis (Bouche), with a rickettsia-like microorganism. American Journal of Tropical Medicine and Hygiene, 43, 400-409.
- AGUIAR, D. M., ZILIANI, T. F., ZHANG, X., MELO, A. L., BRAGA, I. A., WITTER, R., FREITAS, L. C., RONDELLI, A. L., LUIS, M. A., SORTE, E. C., JAUNE, F. W., SANTARÉM, V. A., HORTA, M. C., PESCADOR, C. A., COLODEL, E. M., SOARES, H. S., PACHECO, R. C., ONUMA, S. S., LABRUNA, M. B. & MCBRIDE, J. W., 2014. A novel Ehrlichia genotype strain distinguished by the TRP36 gene naturally infects cattle in Brazil and causes clinical manifestations associated with ehrlichiosis. Ticks and Tick-Borne Diseases, 5, 537-544.
- AGUIRREBENGOA, K., PORTILLO, A., SANTIBÁÑEZ, S., MARÍN, J. J., MONTEJO, M. & OTEO, J. A., 2008. Human Rickettsia sibirica mongolitimonae infection, Spain. Emerging Infectious Diseases, 14, 528.
- AHMED, R., PAUL, S. K., HOSSAIN, M. A., AHMED, S., MAHMUD, M. C., NASREEN, S. A., FERDOUSE, F., SHARMI, R. H., AHAMED, F., GHOSH, S., URUSHIBARA, N., AUNG, M. S. & KOBAYASHI, N., 2016. Molecular detection of Rickettsia felis in humans, cats, and cat fleas in Bangladesh, 2013–2014. Vector-Borne and Zoonotic Diseases, 16, 356-358.
- ALEKSEEV, A. N., DUBININA, H. V., VAN DE POL, I. & SCHOULS, L. M., 2001. Identification of Ehrlichia spp. and Borrelia burgdorferi in Ixodes ticks in the Baltic regions of Russia. Journal of Clinical Microbiology, 39, 2237-2242.
- ALLSOPP, M. T., VISSER, E., DU PLESSIS, J., VOGEL, S. & ALLSOPP, B., 1997. Different organisms associated with heartwater as shown by analysis of 16S ribosomal RNA gene sequences. Veterinary Parasitology, 71, 283-300.
- ALTHAUS, F., GREUB, G., RAOULT, D. & GENTON, B., 2010. African tick-bite fever: a new entity in the differential diagnosis of multiple eschars in travelers. Description of five cases imported from South Africa to Switzerland. International Journal of Infectious Diseases 14, e274-e276.
- ANDERSON, B. E., DAWSON, J. E., JONES, D. C. & WILSON, K. H., 1991. Ehrlichia chaffeensis, a new species associated with human ehrlichiosis. Journal of Clinical Microbiology, 29, 2838-2842.
- ANDERSON, B. E., GREENE, C. E., JONES, D. C. & DAWSON, J. E., 1992. Ehrlichia ewingii sp. nov., the etiologic agent of canine granulocytic ehrlichiosis. International Journal of Systematic Bacteriology, 42, 299-302.
- ANDERSON, B. E., SIMS, K. G., OLSON, J. G., CHILDS, J. E., PIESMAN, J. F., HAPP, C. M., MAUPIN, G. O. & JOHNSON, B. J., 1993. Amblyomma americanum: a potential vector of human ehrlichiosis. American Journal of Tropical Medicine and Hygiene, 49, 239-44.
- ANDERSSON, J. & ANDERSSON, S., 2000. A centruy of typhus, lice and Rickettsia. Research in Microbiology, 151, 143-150.
- ANDERSSON, M., TURCITU, M. A., STEFANACHE, M., TAMBA, P., BARBUCEANU, F. & CHITIMIA, L., 2013. First evidence of Anaplasma platys and Hepatozoon canis co-infection in a dog from Romania–a case report. Ticks and Tick-borne Diseases, 4, 317-319.
- ANGEL-MORENO, A., BOLANOS, M., SANTAN, A. E. & PEREZ-ARELLANO, J., 2006. Murine typhus imported from Senegal in a travelling immigrant. Enfermedades Infecciosas y Microbiologia Clinica 24, 406-407.
- ANGELAKIS, E., PULCINI, C., WATON, J., IMBERT, P., SOCOLOVSCHI, C., EDOUARD, S., DELLAMONICA, P. & RAOULT, D., 2010. Scalp eschar and neck lymphadenopathy caused by Bartonella henselae after tick bite. Clinical Infectious Diseases, 50, 549-551.
- ANSTEY, N. M., TISSOT DUPONT, H., HAHN, C. G., MWAIKAMBO, E. D., MCDONALD, M. I., RAOULT, D. & SEXTON, D. J., 1997. Seroepidemiology of Rickettsia typhi, spotted fever group rickettsiae, and Coxiella burnetti infection in pregnant women from urban Tanzania. American Journal of Tropical Medicine and Hygiene 57, 187-189.
- ANTOGNONI, M. T., VERONESI, F., MORGANTI, G., MANGILI, V., FRUGANTI, G. & MIGLIO, A., 2014. Natural infection of Anaplasma platys in dogs from Umbria region (Central Italy). Veterinaria Italiana, 50, 49-56.
- ANZIANI, O. S., EWING, S. A. & BARKER, R. W., 1990. Experimental transmission of a granulocytic form of the tribe Ehrlichieae by Dermacentor variabilis and Amblyomma americanum to dogs. American Journal of Veterinary Research, 51, 929-931.
- ARRAGA-ALVARADO, C. M., QUROLLO, B. A., PARRA, O. C., BERRUETA, M. A., HEGARTY, B. C. & BREITSCHWERDT, E. B., 2014. Molecular evidence of Anaplasma platys infection in two women from Venezuela. American Journal of Tropical Medicine and Hygiene, 91, 1161-1165.
- ATIF, F. A., 2015. Anaplasma marginale and Anaplasma phagocytophilum: Rickettsiales pathogens of veterinary and public health significance. Parasitology Research, 114, 3941-3957.
- AUBRY, P. & GEALE, D., 2011. A review of bovine anaplasmosis. Transboundary and Emerging Diseases, 58, 1-30.
- AZZAG, N., PETIT, E., GANDOIN, C., BOUILLIN, C., GHALMI, F., HADDAD, N. & BOULOUIS, H. J., 2015. Prevalence of select vector-borne pathogens in stray and client-owned dogs from Algiers. Comparative Immunology, Microbiology and Infectious Diseases, 38, 1-7.
- BAKKEN, J. S. & DUMLER, J. S., 2006. Clinical diagnosis and treatment of human granulocytotropic anaplasmosis. Annals of the New York Academy of Sciences, 1078, 236-247.
- BAKKEN, J. S. & DUMLER, S., 2008. Human granulocytic anaplasmosis. Infectious Disease Clinics of North America, 22, 433-448.
- BALDRIDGE, G. D., SCOLES, G., BURKHARDT, N. Y., SCHLOEDER, B., KURTTI, T. J. & MUNDERLOH, U. G., 2009. Transovarial transmission of Francisella-like endosymbionts and Anaplasma phagocytophilum variants in Dermacentor albipictus (Acari: Ixodidae). Journal of Medical Entomology, 46, 625-632.
- BARTON, L. L. & FOY, T. M., 1989. Ehrlichia canis infection in a child. Pediatrics, 84, 580-582.
- BECHAH, Y., SOCOLOVSCHI, C. & RAOULT, D., 2011. Identification of rickettsial infections by using cutaneous swab specimens and PCR. Emerging Infectious Diseases 17, 83.
- BELKAHIA, H., BEN SAID, M., ALBERTI, A., ABDI, K., ISSAOUI, Z., HATTAB, D., GHARBI, M. & MESSADI, L., 2015. First molecular survey and novel genetic variants’ identification of Anaplasma marginale, A. centrale and A. bovis in cattle from Tunisia. Infection, Genetics and Evolution, 34, 361-371.
- BELKAHIA, H., BEN SAID, M., EL MABROUK, N., SAIDANI, M., CHERNI, C., BEN HASSEN, M., BOUATTOUR, A. & MESSADI, L., 2017. Seasonal dynamics, spatial distribution and genetic analysis of Anaplasma species infecting small ruminants from Northern Tunisia. Infection, Genetics and Evolution, 54, 66-73.
- BELKAHIA, H., BEN SAID, M., EL MABROUK, N., SAIDANI, M., CHERNI, C., BEN HASSEN, M., BOUATTOUR, A. & MESSADI, L., 2017. Spatio-temporal variations and genetic diversity of Anaplasma spp. in cattle from the North of Tunisia. Veterinary Microbiology 208, 223-230.
- BELKAHIA, H., SAID, M. B., SAYAHI, L., ALBERTI, A. & MESSADI, L., 2015. Detection of novel strains genetically related to Anaplasma platys in Tunisian one-humped camels (Camelus dromedarius). Journal of Infection in Developing Countries, 9, 1117-1125.
- BELTRAME, A., ANGHEBEN, A., CASOLARI, S., CASTELLI, F., MAGNANI, G., GAIERA, G., BRILLO, F., CATTANI, G., ANSELMI, M., TOMASONI, L., PRATI, F., NORBERTO, C., SOCOLOVSCHI, C., BISOFFI, Z., RAOULT, D., PAROLA, P., DAVOUST, B. & RAOULT, D., 2012. Imported rickettsioses in Italy. Travel Medicine and Infectious Disease, 10, 201-204.
- BEN SAID, M., BELKAHIA, H., ALBERTI, A., ZOBBA, R., BOUSRIH, M., YAHIAOUI, M., DAALOUL-JEDIDI, M., MAMLOUK, A., GHARBI, M. & MESSADI, L., 2015. Molecular survey of Anaplasma species in small ruminants reveals the presence of novel strains closely related to A. phagocytophilum in Tunisia. Vector-Borne and Zoonotic Diseases, 15, 580-590.
- BEN SAID, M., BELKAHIA, H., EL MABROUK, N., SAIDANI, M., ALBERTI, A., ZOBBA, R., CHERIF, A., MAHJOUB, T., BOUATTOUR, A. & MESSADI, L., 2017. Anaplasma platys-like strains in ruminants from Tunisia. Infection, Genetics and Evolution, 49, 226-233.
- BEN SAID, M., BELKAHIA, H., EL MABROUK, N., SAIDANI, M., BEN HASSEN, M., ALBERTI, A., ZOBBA, R., BOUATTOUR, S., BOUATTOUR, A. & MESSADI, L., 2017. Molecular typing and diagnosis of Anaplasma spp. closely related to Anaplasma phagocytophilum in ruminants from Tunisia. Ticks and Tick-borne diseases, 8, 412-422.
- BEN SAID, M., BELKAHIA, H., HÉNI, M. M., BOUATTOUR, A., GHORBEL, A., GHARBI, M., ZOUARI, A., DARGHOUTH, M. A. & MESSADI, L., 2014. Seroprevalence of Anaplasma phagocytophilum in well-maintained horses from Northern Tunisia. Tropical Biomedicine, 31, 432-440.
- BEN SAID, M., BELKAHIA, H., KARAOUD, M., BOUSRIH, M., YAHIAOUI, M., DAALOUL-JEDIDI, M. & MESSADI, L., 2015. First molecular survey of Anaplasma bovis in small ruminants from Tunisia. Veterinary Microbiology, 179, 322-326.
- BEN SAID, M., BELKAHIA, H. & MESSADI, L., 2018. Anaplasma spp. in North Africa: A review on molecular epidemiology, associated risk factors and genetic characteristics. Ticks and Tick-borne Diseases.
- BERGGOETZ, M., SCHMID, M., STON, D., WYSS, V., CHEVILLON, C., PRETORIUS, A. M. & GERN, L., 2014. Tick-borne pathogens in the blood of wild and domestic ungulates in South Africa: interplay of game and livestock. Ticks and Tick-borne Diseases, 5, 166-175.
- BIGGS, H. M., 2016. Diagnosis and management of tickborne rickettsial diseases: Rocky Mountain spotted fever and other spotted fever group rickettsioses, ehrlichioses, and anaplasmosis—United States. MMWR, Recommendations and Reports, 65.
- BITAM, I., 2012. Vectors of rickettsiae in Africa. Ticks and Tick-Borne Diseases, 3, 382-386.
- BITAM, I., BAZIZ, B., KERNIF, T., HARRAT, Z., PAROLA, P. & RAOULT, D., 2009. Molecular detection of Rickettsia typhi and Rickettsia felis in fleas from Algeria. Clinical Microbiology and Infection, 15, 255-256.
- BITAM, I., PAROLA, P., MATSUMOTO, K., ROLAIN, J. M., BAZIZ, B., BOUBIDI, S. C., HARRAT, Z., BELKAID, M. & RAOULT, D., 2006. First molecular detection of R. conorii, R. aeschlimannii, and R. massiliae in ticks from Algeria. Annals of the New York Academy of Sciences, 1078, 368-372.
- BJÖERSDORFF, A., SVENDENIUS, L., OWENS, J. & MASSUNG, R. F., 1999. Feline granulocytic ehrlichiosis‐a report of a new clinical entity and characterisation of the infectious agent. Journal of Small Animal Practice, 40, 20-24.
- BLANTON, L. S., IDOWU, B. M., TATSCH, T. N., HENDERSON, J. M., BOUYER, D. H. & WALKER, D. H., 2016. Opossums and cat fleas: new insights in the ecology of murine typhus in Galveston, Texas. American Journal of Tropical Medicine and Hygiene, 95, 457-461.
- BOTELHO-NEVERS, E., SOCOLOVSCHI, C., RAOULT, D. & PAROLA, P., 2012. Treatment of Rickettsia spp. infections: a review. Expert Review of Anti-Infective Therapy, 10, 1425-1437.
- BOUYER, D. H., STENOS, J., CROCQUET-VALDES, P., MORON, C. G., POPOV, V. L., ZAVALA-VELAZQUEZ, J. E., FOIL, L. D., STOTHARD, D. R., AZAD, A. F. & WALKER, D. H., 2001. Rickettsia felis: molecular characterization of a new member of the spotted fever group. International Journal of Systematic and Evolutionary Microbiology 51, 339-347.
- BOUZOURAA, T., RENÉ-MARTELLET, M., CHÊNE, J., ATTIPA, C., LEBERT, I., CHALVET-MONFRAY, K., CADORÉ, J. L., HALOS, L. & CHABANNE, L., 2016. Clinical and laboratory features of canine Anaplasma platys infection in 32 naturally infected dogs in the Mediterranean basin. Ticks and Tick-borne Diseases, 7, 1256-1264.
- BREITSCHWERDT, E. B., HEGARTY, B. C. & HANCOCK, S. I., 1998. Sequential evaluation of dogs naturally infected with Ehrlichia canis, Ehrlichia chaffeensis, Ehrlichia equi, Ehrlichia ewingii, or Bartonella vinsonii. Journal of Clinical Microbiology, 36, 2645-2651.
- BREITSCHWERDT, E. B., HEGARTY, B. C., QUROLLO, B. A., SAITO, T. B., MAGGI, R. G., BLANTON, L. S. & BOUYER, D. H., 2014. Intravascular persistence of Anaplasma platys, Ehrlichia chaffeensis, and Ehrlichia ewingii DNA in the blood of a dog and two family members. Parasites and Vectors, 7, 298.
- BRODIE, T., HOLMES, P. & URQUHART, G. M., 1986. Some aspects of tick-borne diseases of British sheep. Veterinary Record 118, 415-418.
- BUCHAU, A., WURTHNER, J., BYLAITE, M., KUKOVA, G., RUZICKA, T. & REIFENBERGER, J., 2006. Rickettsiosis after holiday in Swaziland. Hautarzt, 57, 328-330.
- BULLER, R. S., ARENS, M., HMIEL, S. P., PADDOCK, C. D., SUMNER, J. W., RIKHISA, Y., UNVER, A., GAUDREAULT-KEENER, M., MANIAN, F. A., LIDDELL, A. M., SCHMULEWITZ, N. & STORCH, G. A., 1999. Ehrlichia ewingii, a newly recognized agent of human ehrlichiosis. New England Journal of Medicine, 341, 148-155.
- CAO, W. C., GAO, Y. M., ZHANG, P. H., ZHANG, X. T., DAI, Q. H., DUMLER, J. S., FANG, L. Q. & YANG, H., 2000. Identification of Ehrlichia chaffeensis by nested PCR in ticks from Southern China. Journal of Clinical Microbiology, 38, 2778-2880.
- CAO, W. C., ZHAO, Q. M., ZHANG, P. H., YANG, H., WU, X. M., WEN, B. H., ZHANG, X. T. & HABBEMA, J. D., 2003. Prevalence of Anaplasma phagocytophila and Borrelia burgdorferi in Ixodes persulcatus ticks from northeastern China. American Journal of Tropical Medicine and Hygiene, 68, 547-550.
- CECI, L., IARUSSI, F., GRECO, B., LACINIO, R., FORNELLI, S. & CARELLI, G., 2014. Retrospective study of hemoparasites in cattle in southern Italy by reverse line blot hybridization. Journal of Veterinary Medical Science, 76, 869-875.
- CHAE, J. S., FOLEY, J. E., DUMLER, J. S. & MADIGAN, J. E., 2000. Comparison of the nucleotide sequences of 16S rRNA, 444Ep-ank, and groESL heat shock operon genes in naturally occurring Ehrlichia equi and human granulocytic ehrlichiosis agent isolates from Northern California. Journal of Clinical Microbiology, 38, 1364-1369.
- CHEN, S. M., DUMLER, J. S., BAKKEN, J. S., WALKER, D. H. & DUMLER, J. S., 1994. Identification of a granulocytotropic Ehrlichia species as the etiologic agent of human disease. Journal of Clinical Microbiology, 32, 589-595.
- CHIKEKA, I. & DUMLER, J. S., 2015. Neglected bacterial zoonoses. Clinical Microbiology and Infection, 21, 404-415.
- CHOCHLAKIS, D., IOANNOU, I., SHARIF, L., KOKKINI, S., HRISTOPHI, N., DIMITRIOU, T., TSELENTIS, Y. & PSAROULAKI, A., 2009. Prevalence of Anaplasma sp. in goats and sheep in Cyprus. Vector-Borne and Zoonotic Diseases, 9, 457-463.
- CHRISTOU, C., PSAROULAKI, A., ANTONIOU, M., TOUMAZOS, P., IOANNOU, I., MAZERIS, A., CHOCHLAKIS, D. & TSELENTIS, Y., 2010. Rickettsia typhi and Rickettsia felis in Xenopsylla cheopis and Leptopsylla segnis parasitizing rats in Cyprus. American Journal of Tropical Medicine and Hygiene, 83, 1301-1304.
- CLARK, K. L., 2012. Anaplasma phagocytophilum in small mammals and ticks in northeast Florida. Journal of Vector Ecology, 37, 262-268.
- CLARKE, L. L., BALLWEBER, L. R., ALLEN, K., LITTLE, S. E. & LAPPIN, M. R., 2014. Prevalence of select vector-borne disease agents in owned dogs of Ghana. Journal of the South African Veterinary Association, 85, 1-2.
- COHN, L. A., 2003. Ehrlichiosis and related infections. Veterinary Clinics of North America: Small Animal Practice, 33, 863-884.
- CONOR, A., 1910. Une fièvre éruptive observée en Tunisie. Bulletin de la Société de Pathologie Exotique, 3, 492-496.
- DAHMANI, M., DAVOUST, B., BENTERKI, M. S., FENOLLAR, F., RAOULT, D. & MEDIANNIKOV, O., 2015. Development of a new PCR-based assay to detect Anaplasmataceae and the first report of Anaplasma phagocytophilum and Anaplasma platys in cattle from Algeria. Comparative Immunology, Microbiology and Infectious Diseases, 39, 39-45.
- DAHMANI, M., LOUDAHI, A., MEDIANNIKOV, O., FENOLLAR, F., RAOULT, D. & DAVOUST, B., 2015. Molecular detection of Anaplasma platys and Ehrlichia canis in dogs from Kabylie, Algeria. Ticks and Tick-Borne Diseases, 6, 198-203.
- DAVIDSON, W. R., LOCKHART, J. M., STALLKNECHT, D. E. & HOWERTH, E. W., 1999. Susceptibility of red and gray foxes to infection by Ehrlichia chaffeensis. Journal of Wildlife Diseases, 35, 696-702.
- DAVIDSON, W. R., LOCKHART, J. M., STALLKNECHT, D. E., HOWERTH, E. W., DAWSON, J. E. & RECHAV, Y., 2001. Persistent Ehrlichia chaffeensis infection in white-tailed deer. Journal of Wildlife Disease, 37, 538-546.
- DAWSON, J. E., BIGGIE, K. L., WARNER, C. K., COOKSON, K., JENKINS, S., LEVINE, J. F. & OLSON, J. G., 1996. Polymerase chain reaction evidence of Ehrlichia chaffeensis, an etiologic agent of human ehrlichiosis, in dogs from southeast Virginia. American Journal of Veterinary Research, 57, 1175-1179.
- DAWSON, J. E., CHILDS, J. E., BIGGIE, K. L., MOORE, C., STALLKNECHT, D., SHADDOCK, J., BOUSEMAN, J., HOFMEISTER, E. & OLSON, J. G., 1994. White-tailed deer as a potential reservoir of Ehrlichia spp. Journal of Wildlife Diseases, 30, 162-168.
- DAWSON, J. E. & EWING, S. A., 1992. Susceptibility of dogs to infection with Ehrlichia chaffeensis, causative agent of human ehrlichiosis. American Journal of Veterinary Research, 53, 1322-1327.
- DAWSON, J. E., STALLKNECHT, D. E., HOWERTH, E. W., WARNER, C., BIGGIE, K., DAVIDSON, W. R., LOCKHART, J. M., NETTLES, V. F., OLSON, J. G. & CHILDS, J. E., 1994. Susceptibility of white-tailed deer (Odocoileus virginianus) to infection with Ehrlichia chaffeensis, the etiologic agent of human ehrlichiosis. Journal of Clinical Microbiology, 32, 2725-2728.
- DE SOUSA, R., BARATA, C., VITORINO, L., SANTOS-SILVA, M., CARRAPATO, C., TORGAL, J., WALKER, D. & BACELLAR, F., 2006. Rickettsia sibirica isolation from a patient and detection in ticks, Portugal. Emerging Infectious Diseases, 12, 1103.
- DE SOUSA, R., LOPES DE CARVALHO, I., SANTOS, A. S., BERNARDES, C., MILHANO, N., JESUS, J., MENEZES, D. & NÚNCIO, M. S., 2012. The role of Teira dugesii lizard as potential host for Ixodes ricinus tick-borne pathogens. Applied and Environmental Microbiology, 07945-11.
- DELOS SANTOS, J. R., BOUGHAN, K., BREMER, W. G., RIZZO, B., SCHAEFER, J. J., RIKIHISA, Y., NEEDHAM, G. R., CAPITINI, L. A., ANDERSON, D. E., OGLESBEE, M., EWING, S. A. & STICH, R. W., 2007. Experimental infection of dairy calves with Ehrlichia chaffeensis. Journal of Medical Microbiology, 56, 1660-1668.
- DERGOUSOFF, S. J. & CHILTON, N. B., 2011. Novel genotypes of Anaplasma bovis,“Candidatus Midichloria” sp. and Ignatzschineria sp. in the Rocky Mountain wood tick, Dermacentor andersoni. Veterinary Microbiology, 150, 100-106.
- DIB, L., BITAM, I., BENSOUILAH, M., PAROLA, P. & RAOULT, D., 2009. First description of Rickettsia monacensis in Ixodes ricinus in Algeria. Clinical Microbiology and Infection, 15, 261-262.
- DIEME, C., BECHAH, Y., SOCOLOVSCHI, C., AUDOLY, G., BERENGER, J. M., FAYE, O., RAOULT, D. & PAROLA, P., 2015. Transmission potential of Rickettsia felis infection by Anopheles gambiae mosquitoes. Proceedings of the National Academy of Sciences, 112, 8088-8093.
- DJIBA, M. L., MEDIANNIKOV, O., MBENGUE, M., THIONGANE, Y., MOLEZ, J. F., SECK, M. T., FENOLLAR, F., RAOULT, D. & NDIAYE, M., 2013. Survey of Anaplasmataceae bacteria in sheep from Senegal. Tropical Animal Health and Production, 45, 1557-1561.
- DONATIEN, A. & LESTOQUARD, F., 1936. Existance de la premunition dans la rickettsiose naturelle ou experimentale du chien. Bulletin de la Société de Pathologie Exotique, 29, 378-383.
- DONATIEN, A. & LESTOQUARD, F., 1936. Rickettsia bovis, nouvelle espece pathogene pour le boeuf. Bulletin de la Société de Pathologie Exotique, 29, 1057-1061.
- DUGAN, V. G., LITTLE, S. E., STALLKNECHT, D. E. & BEALL, A. D., 2000. Natural infection of domestic goats with Ehrlichia chaffeensis. Journal of Clinical Microbiology, 38, 448-449.
- DUH, D., PUNDA-POLIC, V., AVSIC-ZUPANC, T., BOUYER, D., WALKER, D. H., POPOV, V. L., JELOVSEK, M., GRACNER, M., TRILAR, T., BRADARIC, N., KURTTI, T. J. & STRUS, J., 2010. Rickettsia hoogstraalii sp. nov., isolated from hard-and soft-bodied ticks. International Journal of Systematic and Evolutionary Microbiology, 60, 977-984.
- DUMLER, J. S., 2012. The biological basis of severe outcomes in Anaplasma phagocytophilum infection. FEMS Immunology and Medical Microbiology, 64, 13-20.
- DUMLER, J. S., BARBET, A. F., BEKKER, C. P., DASCH, G. A., PALMER, G. H., RAY, S. C., RIKIHISA, Y. & RURANGIRWA, F. R., 2001. Reorganization of genera in the families Rickettsiaceae and Anaplasmataceae in the order Rickettsiales: unification of some species of Ehrlichia with Anaplasma, Cowdria with Ehrlichia and Ehrlichia with Neorickettsia, descriptions of six new species combinations and designation of Ehrlichia equi and'HGE agent'as subjective synonyms of Ehrlichia phagocytophila. International Journal of Systematic and Evolutionary Microbiology, 51, 2145-2165.
- EGENVALL, A., HEDHAMMAR, A. & BJÖERSDORFF, A., 1997. Clinical features and serology of 14 dogs affected by granulocytic ehrlichiosis in Sweden. Veterinary Record, 140, 222-226.
- EHOUNOUD, C., FENOLLAR, F., DAHMANI, M., N’GUESSAN, J., RAOULT, D. & MEDIANNIKOV, O., 2017. Bacterial arthropod-borne diseases in West Africa. Acta Tropica, 171, 124-137.
- EHOUNOUD, C. B., YAO, K. P., DAHMANI, M., ACHI, Y. L., AMANZOUGAGHENE, N., KACOU N'DOUBA, A., N'GUESSAN, J. D., RAOULT, D., FENOLLAR, F. & MEDIANNIKOV, O., 2016. Multiple pathogens including potential new species in tick vectors in Côte d’Ivoire. PLoS Neglected Tropical Diseases, 10, e0004367.
- ELDIN, C., MEDIANNIKOV, O., DAVOUST, B., CABRE, O., BARRÉ, N., RAOULT, D. & PAROLA, P., 2011. Emergence of Rickettsia africae, Oceania. Emerging Infectious Diseases, 17, 100.
- EREMEEVA, M. E., OLIVEIRA, A., ROBINSON, J. B., RIBAKOVA, N., TOKAREVICH, N. K. & DASCH, G. A., 2006. Prevalence of bacterial agents in Ixodes persulcatus ticks from the Vologda Province of Russia. Annals of the New York Academy of Sciences, 1078, 291-298.
- ESTRADA-PEÑA, A. & SALMAN, M., 2013. Current limitations in the control and spread of ticks that affect livestock: a review. Agriculture, 3, 221-235.
- FERNÁNDEZ‐SOTO, P., PÉREZ‐SÁNCHEZ, R., ÁLAMO‐SANZ, R. & ENCINAS‐GRANDES, A., 2006. Spotted fever group rickettsiae in ticks feeding on humans in northwestern Spain. Annals of the New York Academy of Sciences, 1078, 331-333.
- FICHTENBAUM, C. J., PETERSON, L. R. & WEIL, G. J., 1993. Ehrlichiosis presenting as a life-threatening illness with features of the toxic shock syndrome. American Journal of Medicine, 95, 351-357.
- FOONGLADDA, S., INTHAWONG, D., KOSITANONT, U. & GAYWEE, J., 2011. Rickettsia, Ehrlichia, Anaplasma, and Bartonella in ticks and fleas from dogs and cats in Bangkok. Vector-Borne and Zoonotic Diseases, 11, 1335-1341.
- FOURIE, J. J., STANNECK, D., LUUS, H. G., BEUGNET, F., WIJNVELD, M. & JONGEJAN, F., 2013. Transmission of Ehrlichia canis by Rhipicephalus sanguineus ticks feeding on dogs and on artificial membranes. Veterinary Parasitology, 197, 595-603.
- FOURNIER, P. E., GOURIET, F., BROUQUI, P., LUCHT, F. & RAOULT, D., 2005. Lymphangitis-associated rickettsiosis, a new rickettsiosis caused by Rickettsia sibirica mongolotimonae: seven new cases and review of the literature. Clinical Infectious Diseases, 40, 1435-1444.
- FRANZÉN, P., ASPAN, A., EGENVALL, A., GUNNARSSON, A., ABERG, L. & PRINGLE, J., 2005. Acute clinical, hematologic, serologic, and polymerase chain reaction findings in horses experimentally infected with a European strain of Anaplasma phagocytophilum. Journal of Veterinary Internal Medicine, 19, 232-239.
- FRANZÉN, P., BERG, A., ASPAN, A., GUNNARSSON, A. & PRINGLE, J., 2007. Death of a horse infected experimentally with Anaplasma phagocytophilum. Veterinary Record, 160, 122-125.
- GAJADHAR, A. A., LOBANOV, V., SCANDRETT, W. B., CAMPBELL, J. & AL-ADHAMI, B., 2010. A novel Ehrlichia genotype detected in naturally infected cattle in North America. Veterinary Parasitology, 173, 324-329.
- GARCIA‐PEREZ, A. L., BARANDIKA, J., OPORTO, B., POVEDANO, I. & JUSTE, R. A., 2003. Anaplasma phagocytophila as an abortifacient agent in sheep farms from northern Spain. Annals of the New York Academy of Sciences, 990, 429-432.
- GASTELLIER, L., LANTERNIER, F., RENVOISÉ, A., RIVIÈRE, S., RAOULT, D., LORTHOLARY, O. & LECUIT, M., 2014. Noneruptive fever revealing murine typhus in a traveler returning from Tunisia. Journal of Travel Medicine, 22, 67-69.
- GAUNT, S., BAKER, D. & BABIN, S., 1990. Platelet aggregation studies in dogs with acute Ehrlichia platys infection. American Journal of Veterinary Research, 51, 290-293.
- GHAFAR, M. W. & AMER, S. A., 2012. Prevalence and first molecular characterization of Anaplasma phagocytophilum, the agent of human granulocytic anaplasmosis, in Rhipicephalus sanguineus ticks attached to dogs from Egypt. Journal of Advanced Research, 3, 189-194.
- GIAMMANCO, G. M., VITALE, G., MANSUETO, S., CAPRA, G., CALECA, M. P. & AMMATUNA, P., 2005. Presence of Rickettsia conorii subsp. israelensis, the causative agent of Israeli spotted fever, in Sicily, Italy, ascertained in a retrospective study. Journal of Clinical Microbiology, 43, 6027-6031.
- GILLESPIE, J. J., AMMERMAN, N. C., BEIER-SEXTON, M., SOBRAL, B. S. & AZAD, A. F., 2009. Louse-and flea-borne rickettsioses: biological and genomic analyses. Veterinary Research, 40, 1.
- GOETHERT, H. K. & TELFORD, S. R., 2003. Enzootic transmission of Anaplasma bovis in Nantucket cottontail rabbits. Journal of Clinical Microbiology, 41, 3744-3747.
- GOODMAN, R. A., HAWKINS, E. C., OLBY, N. J., GRINDEM, C. B., HEGARTY, B. & BREITSCHWERDT, E. B., 2003. Molecular identification of Ehrlichia ewingii infection in dogs: 15 cases (1997-2001). Journal of the American Veterinary Medical Association, 222, 1102-1107.
- GORDON, W., BROWNLEE, A. & WILSON, D., 1940. Studies in louping-ill, tick-borne fever and scrapie. Presented at Proceedings: 3rd International Congress of Microbiology.
- GORDON, W., BROWNLEE, A., WILSON, D. & MACLEOD, J., 1932. " Tick-borne Fever"(A hitherto undescribed Disease of Sheep). Journal of Comparative Pathology, 45.
- GÖTSCH, S., LESCHNIK, M., DUSCHER, G., BURGSTALLER, J., WILLE-PIAZZAI, W. & JOACHIM, A., 2009. Ticks and haemoparasites of dogs from Praia, Cape Verde. Veterinary Parasitology, 166, 171-174.
- GROVA, L., OLESEN, I., STEINSHAMN, H. & STUEN, S., 2011. Prevalence of Anaplasma phagocytophilum infection and effect on lamb growth. Acta Veterinaria Scandinavica, 53, 30.
- GROVES, M. G., DENNIS, G. L., AMYX, H. L. & HUXSOLL, D. L., 1975. Transmission of Ehrlichia canis to dogs by ticks (Rhipicephalus sanguineus). American Journal of Veterinary Research, 36, 937-940.
- HARKESS, J., 1991. Ehrlichiosis. Infectious Disease Clinics of North America, 5, 37-51.
- HARRUS, S., PERLMAN‐AVRAHAMI, A., MUMCUOGLU, K., MORICK, D. & BANETH, G., 2011. Molecular detection of Rickettsia massiliae, Rickettsia sibirica mongolitimonae and Rickettsia conorii israelensis in ticks from Israel. Clinical Microbiology and Infection, 17, 176-180.
- HARRUS, S., WANER, T., AIZENBERG, I., FOLEY, J. E., POLAND, A. M. & BARK, H., 1998. Amplification of ehrlichial DNA from dogs 34 months after infection with Ehrlichia canis. Journal of Clinical Microbiology, 36, 73-76.
- HARVEY, J. W., SIMPSON, C. F. & GASKIN, J. M., 1978. Cyclic thrombocytopenia induced by a Rickettsia-like agent in dogs. Journal of Infectious Diseases, 137, 182-188.
- HEIKKILÄ, H. M., BONDARENKO, A., MIHALKOV, A., PFISTER, K. & SPILLMANN, T., 2010. Anaplasma phagocytophilum infection in a domestic cat in Finland: case report. Acta Veterinaria Scandinavica, 52, 62.
- HEITMAN, K. N., DAHLGREN, F. S., DREXLER, N. A., MASSUNG, R. F. & BEHRAVESH, C. B., 2016. Increasing incidence of ehrlichiosis in the United States: a summary of national surveillance of Ehrlichia chaffeensis and Ehrlichia ewingii infections in the United States, 2008–2012. American Journal of Tropical Medicine and Hygiene, 94, 52-60.
- HERRON, M. J., NELSON, C. M., LARSON, J., SNAPP, K. R., KANSAS, G. S. & GOODMAN, J. L., 2000. Intracellular parasitism by the human granulocytic ehrlichiosis bacterium through the P-selectin ligand, PSGL-1. Science, 288, 1653-1656.
- HII, S. F., KOPP, S. R., ABDAD, M. Y., THOMPSON, M. F., O'LEARY, C. A., REES, R. L. & TRAUB, R. J., 2011. Molecular evidence supports the role of dogs as potential reservoirs for Rickettsia felis. Vector-Borne and Zoonotic Diseases, 11, 1007-1012.
- HII, S. F., KOPP, S. R., THOMPSON, M., O'LEARY, C. A., REES, R. L. & TRAUB, R. J., 2011. Molecular evidence of Rickettsia felis infection in dogs from northern territory, Australia. Parasites and Vectors, 4, 198.
- HOLDEN, K., BOOTHBY, J. T., ANAND, S. & MASSUNG, R. F., 2003. Detection of Borrelia burgdorferi, Ehrlichia chaffeensis, and Anaplasma phagocytophilum in ticks (Acari: Ixodidae) from a coastal region of California. Journal of Medical Entomology, 40, 534-539.
- HORNOK, S., ABICHU, G., TAKÁCS, N., GYURANECZ, M., FARKAS, R., FERNÁNDEZ DE MERA, I. G. & DE LA FUENTE, J., 2016. Molecular screening for Anaplasmataceae in ticks and tsetse flies from Ethiopia. Acta Veterinaria Hungarica, 64, 65-70.
- HORNOK, S., MELI, M. L., PERRETEN, A., FARKAS, R., WILLI, B., BEUGNET, F., LUTZ, H. & HOFMANN-LEHMANN, R., 2010. Molecular investigation of hard ticks (Acari: Ixodidae) and fleas (Siphonaptera: Pulicidae) as potential vectors of rickettsial and mycoplasmal agents. Veterinary Microbiology, 140, 98-104.
- HUEBNER, R. J., JELLISON, W. L. & ARMSTRONG, C. H., 1947. Rickettsialpox: A newly recognized rickettsial disease: V. Recovery of Rickettsia akari from a house mouse (Mus musculus). Public Health Reports (1896-1970), 777-780.
- INOKUMA, H., OHASHI, M., JILINTAI., TANABE, S. & MIYAHARA, K., 2007. Prevalence of tick-borne Rickettsia and Ehrlichia in Ixodes persulcatus and Ixodes ovatus in Tokachi district, Eastern Hokkaido, Japan. Journal of Veterinary Medical Science, 69, 661-664.
- JADO, I., OTEO, J. A., ALDÁMIZ, M., GIL, H., ESCUDERO, R., IBARRA, V., PORTU, J., PORTILLO, A., LEZAUN, M. J., GARCÍA-AMIL, C., RODRÍGUEZ-MORENO, I. & ANDA, P., 2007. Rickettsia monacensis and human disease, Spain. Emerging Infectious Diseases, 13, 1405.
- JENKINS, A., KRISTIANSEN, B. E., ALLUM, A. G., AAKRE, R. K., STRAND, L., KLEVELAND, E. J., VAN DE POL, I. & SCHOULS, L., 2001. Borrelia burgdorferi Sensu Lato andEhrlichia spp. in Ixodes Ticks from Southern Norway. Journal of Clinical Microbiology, 39, 3666-3671.
- JENSENIUS, M., DAVIS, X., VON SONNENBURG, F., SCHWARTZ, E., KEYSTONE, J. S., LEDER, K., LOPÉZ-VÉLÉZ, R., CAUMES, E., CRAMER, J. P., CHEN, L., PAROLA, P. & NETWORK., G. S. S., 2009. Multicenter GeoSentinel analysis of rickettsial diseases in international travelers, 1996–2008. Emerging Infectious Diseases, 15, 1791.
- JENSENIUS, M., FOURNIER, P. E., KELLY, P., MYRVANG, B. & RAOULT, D., 2003. African tick bite fever. Lancet Infectious Diseases, 3, 557-564.
- JENSENIUS, M., FOURNIER, P. E., VENE, S., HOEL, T., HASLE, G., HENRIKSEN, A. Z., HELLUM, K. B., RAOULT, D., MYRVANG, B. & GROUP., N. A. T. B. F. S., 2003. African tick bite fever in travelers to rural sub-Equatorial Africa. Clinical Infectious Diseases, 36, 1411-1417.
- JIANG, J., YOU, B. J., LIU, E., APTE, A., YARINA, T. R., MYERS, T. E., LEE, J. S., FRANCESCONI, S. C., O'GUINN, M. L., TSERTSVADZE, N., VEPHKHVADZE, N., BABUADZE, G., SIDAMONIDZE, K., KOKHREIDZE, M., DONDUASHVILI, M., ONASHVILI, T., ISMAYILOV, A., AGAYEV, N., ALIYEV, M., MUTTALIBOV, N. & RICHARDS, A. L., 2012. Development of three quantitative real-time PCR assays for the detection of Rickettsia raoultii, Rickettsia slovaca, and Rickettsia aeschlimannii and their validation with ticks from the country of Georgia and the Republic of Azerbaijan. Ticks and Tick-Borne Diseases, 3, 327-331.
- JILINTAI., SEINO, N., HAYAKAWA, D., SUZUKI, M., HATA, H., KONDO, S., MATSUMOTO, K., YOKOYAMA, N. & INOKUMA, H., 2009. Molecular survey for Anaplasma bovis and Anaplasma phagocytophilum infection in cattle in a pastureland where sika deer appear in Hokkaido, Japan. Japanese Journal of Infectious Diseases, 62, 73-75.
- JOHNSON, E. M., EWING, S. A., BARKER, R. W., FOX, J. C., CROW, D. W. & KOCAN, K. M., 1998. Experimental transmission of Ehrlichia canis (Rickettsiales: Ehrlichieae) by Dermacentor variabilis (Acari: Ixodidae). Veterinary Parasitology, 74, 277-288.
- KAMANI, J., BANETH, G., APANASKEVICH, D., MUMCUOGLU, K. & HARRUS, S., 2015. Molecular detection of Rickettsia aeschlimannii in Hyalomma spp. ticks from camels (Camelus dromedarius) in Nigeria, West Africa. Medical and Veterinary Entomology, 29, 205-209.
- KAMANI, J., BANETH, G., MUMCUOGLU, K. Y., WAZIRI, N. E., EYAL, O., GUTHMANN, Y. & HARRUS, S., 2013. Molecular detection and characterization of tick-borne pathogens in dogs and ticks from Nigeria. PLoS Neglected Tropical Diseases, 7, e2108.
- KANG, Y. J., DIAO, X. N., ZHAO, G. Y., CHEN, M. H., XIONG, Y., SHI, M., FU, W. M., GUO, Y. J., PAN, B., CHEN, X. P., HOLMES, E. C., GILLESPIE, J. J., DUMLER, S. J. & ZHANG, Y. Z., 2014. Extensive diversity of Rickettsiales bacteria in two species of ticks from China and the evolution of the Rickettsiales. BMC Evolutionary Biology, 14, 167.
- KAWAHARA, M., ITO, T., SUTO, C., SHIBATA, S., RIKIHISA, Y., HATA, K. & HIRAI, K., 1999. Comparison of Ehrlichia muris strains isolated from wild mice and ticks and serologic survey of humans and animals with E. muris as antigen. Journal of Clinical Microbiology, 37, 1123-1129.
- KAWAHARA, M., RIKIHISA, Y., LIN, Q., ISOGAI, E., TAHARA, K., ITAGAKI, A., HIRAMITSU, Y. & TAJIMA, T., 2006. Novel genetic variants of Anaplasma phagocytophilum, Anaplasma bovis, Anaplasma centrale, and a novel Ehrlichia sp. in wild deer and ticks on two major islands in Japan. Applied and Environmental Microbiology, 72, 1102-1109.
- KELLY, D. J., RICHARDS, A. L., TEMENAK, J., STRICKMAN, D. & DASCH, G. A., 2002. The past and present threat of rickettsial diseases to military medicine and international public health. Clinical Infectious Diseases, 34, S145-S169.
- KELLY, P., LUCAS, H., BEATI, L., YOWELL, C., MAHAN, S. & DAME, J., 2010. Rickettsia africae in Amblyomma variegatum and domestic ruminants on eight Caribbean islands. Journal of Parasitology, 96, 1086-1088.
- KELLY, P. J., MASON, P., MANNING, T. & SLATER, S., 1991. Role of cattle in the epidemiology of tick-bite fever in Zimbabwe. Journal of Clinical Microbiology, 29, 256-259.
- KERNIF, T., MESSAOUDENE, D., OUAHIOUNE, S., PAROLA, P., RAOULT, D. & BITAM, I., 2012. Spotted fever group rickettsiae identified in Dermacentor marginatus and Ixodes ricinus ticks in Algeria. Ticks and Tick-Borne Diseases, 3, 380-381.
- KERNIF, T., SOCOLOVSCHI, C., BITAM, I., RAOULT, D. & PAROLA, P., 2012. Vector-borne rickettsioses in North Africa. Infectious Disease Clinics, 26, 455-478.
- KHATAT, S. E., KHALLAAYOUNE, K., ERRAFYK, N., VAN GOOL, F., DUCHATEAU, L., DAMINET, S., KACHANI, M., EL AMRI, H., AZRIB, R. & SAHIBI, H., 2017. Detection of Anaplasma spp. and Ehrlichia spp. anibodies, and Dirofilaria immitis antigens in dogs from seven locations of Morocco. Veterinary Parasitology, 239, 86-89.
- KHATAT, S. E., SAHIBI, H., HING, M., ALAOUI MOUSTAIN, I., EL AMRI, H., BENAJIBA, M., KACHANI, M., DUCHATEAU, L. & DAMINET, S., 2016. Human exposure to Anaplasma phagocytophilum in two cities of northwestern Morocco. PloS One, 11, e0160880.
- KHROUF, F., M'GHIRBI, Y., ZNAZEN, A., JEMAA, M. B., HAMMAMI, A. & BOUATTOUR, A., 2014. Detection of Rickettsia in Rhipicephalus sanguineus ticks and Ctenocephalides felis fleas from southeastern Tunisia by reverse line blot assay. Journal of Clinical Microbiology, 52, 268-274.
- KHROUF, F., SELLAMI, H., ELLEUCH, E., HATTAB, Z., AMMARI, L., KHALFAOUI, M., SOUISSI, J., HARRABI, H., M'GHIRBI, Y., TIOUIRI, H., BEN JEMAA, M., HAMMAMI, A., LETAIEF, A., BOUATTOUR, A. & ZNAZEN, A., 2016. Molecular diagnosis of Rickettsia infection in patients from Tunisia. Ticks and Tick-Borne Diseases, 7, 653-656.
- KIM, C. M., KIM, M. S., PARK, M. S., PARK, J. H. & CHAE, J. S., 2003. Identification of Ehrlichia chaffeensis, Anaplasma phagocytophilum, and A. bovis in Haemaphysalis longicornis and Ixodes persulcatus ticks from Korea. Vector-Borne and Zoonotic Diseases, 3, 17-26.
- KIM, C. M., YI, Y. H., YU, D. H., LEE, M. J., CHO, M. R., DESAI, A. R., SHRINGI, S., KLEIN, T. A., KIM, H. C., SONG, J. W., BAEK, L. J., CHONG, S. T., O'GUINN, M. L., LEE, J. S., LEE, I. Y., PARK, J. H., FOLEY, J. & CHAE, J. S., 2006. Tick-borne rickettsial pathogens in ticks and small mammals in Korea. Applied and Environmental Microbiology, 72, 5766-5776.
- KIRCHNER, M., BRUNNER, A., EDELHOFER, R. & JOACHIM, A., 2008. Vector-borne parasites of dogs on the Islands of Cabo Verde. Wiener Klinische Wochenschrift, 120, 49-53.
- KLEINERMAN, G., BANETH, G., MUMCUOGLU, K. Y., VAN STRATEN, M., BERLIN, D., APANASKEVICH, D. A., ABDEEN, Z., NASEREDDIN, A. & HARRUS, S., 2013. Molecular detection of Rickettsia africae, Rickettsia aeschlimannii, and Rickettsia sibirica mongolitimonae in camels and Hyalomma spp. ticks from Israel. Vector-Borne and Zoonotic Diseases, 13, 851-856.
- KO, S., KIM, H. C., YANG, Y. C., CHONG, S. T., RICHARDS, A. L., SAMES, W. J., KLEIN, T. A., KANG, J. G. & CHAE, J. S., 2011. Detection of Rickettsia felis and Rickettsia typhi and seasonal prevalence of fleas collected from small mammals at Gyeonggi Province in the Republic of Korea. Vector-Borne and Zoonotic Diseases, 11, 1243-1251.
- KOCAN, A. A., LEVESQUE, G. C., WHITWORTH, L. C., MURPHY, G. L., EWING, S. A. & BARKER, R. W., 2000. Naturally occurring Ehrlichia chaffeensis infection in coyotes from Oklahoma. Emerging Infectious Diseases, 6, 477-480.
- KOLO, A. O., SIBEKO-MATJILA, K. P., MAINA, A. N., RICHARDS, A. L., KNOBEL, D. L. & MATJILA, P. T., 2016. Molecular detection of zoonotic rickettsiae and Anaplasma spp. in domestic dogs and their ectoparasites in Bushbuckridge, South Africa. Vector-Borne and Zoonotic Diseases, 16, 245-252.
- KRAKOWETZ, C. N., DIBERNARDO, A., LINDSAY, L. R. & CHILTON, N. B., 2014. Two Anaplasma phagocytophilum strains in Ixodes scapularis ticks, Canada. Emerging Infectious Diseases, 20, 2064.
- KRAMER, V. L., RANDOLPH, M. P., HUI, L. T., IRWIN, W. E., GUTIERREZ, A. G. & VUGIA, D. J., 1999. Detection of the agents of human ehrlichioses in ixodid ticks from California. American Journal of Tropical Medicine and Hygiene, 60, 62-65.
- KUO, C. C., SHU, P. Y., MU, J. J. & WANG, H. C., 2015. High prevalence of Rickettsia spp. infections in small mammals in Taiwan. Vector-Borne and Zoonotic Diseases, 15, 13-20.
- LANE, R. S., MUN, J., PERIBÁÑEZ, M. A. & FEDOROVA, N., 2010. Differences in prevalence of Borrelia burgdorferi and Anaplasma spp. infection among host-seeking Dermacentor occidentalis, Ixodes pacificus, and Ornithodoros coriaceus ticks in northwestern California. Ticks and Tick-Borne Diseases, 1, 159-167.
- LAUZI, S., MAIA, J. P., EPIS, S., MARCOS, R., PEREIRA, C., LUZZAGO, C., SANTOS, M., PUENTE-PAYO, P., GIORDANO, A., PAJORO, M., SIRONI, G. & FAUSTINO, A., 2016. Molecular detection of Anaplasma platys, Ehrlichia canis, Hepatozoon canis and Rickettsia monacensis in dogs from Maio Island of Cape Verde archipelago. Ticks and Tick-Borne Diseases, 7, 964-969.
- LBACHA, H. A., ZOUAGUI, Z., ALALI, S., RHALEM, A., PETIT, E., DUCROTOY, M. J., BOULOUIS, H. & MAILLARD, R., 2017. Candidatus anaplasma camelii in one-humped camels (Camelus dromedarius) in Morocco: a novel and emerging Anaplasma species? Infectious Diseases of Poverty, 6, 1.
- LEE, M., YU, D., YOON, J., LI, Y., LEE, J. & PARK, J., 2009. Natural co-infection of Ehrlichia chaffeensis and Anaplasma bovis in a deer in South Korea. Journal of Veterinary Medical Science, 71, 101-103.
- LEE, S. O., NA, D. K., KIM, C. M., LI, Y. H., CHO, Y. H., PARK, J. H., LEE, J. H., EO, S. K., KLEIN, T. A. & CHAE, J. S., 2005. Identification and prevalence of Ehrlichia chaffeensis infection in Haemaphysalis longicornis ticks from Korea by PCR, sequencing and phylogenetic analysis based on 16S rRNA gene. Journal of Veterinary Medical Science, 6, 151-155.
- LEIBY, D. A. & GILL, J. E., 2004. Transfusion-transmitted tick-borne infections: a cornucopia of threats. Transfusion Medicine Reviews, 18, 293-306.
- LEULMI, H., AOUADI, A., BITAM, I., BESSAS, A., BENAKHLA, A., RAOULT, D. & PAROLA, P., 2016. Detection of Bartonella tamiae, Coxiella burnetii and rickettsiae in arthropods and tissues from wild and domestic animals in northeastern Algeria. Parasites and Vectors, 9, 27.
- LEULMI, H., SOCOLOVSCHI, C., LAUDISOIT, A., HOUEMENOU, G., DAVOUST, B., BITAM, I., RAOULT, D. & PAROLA, P., 2014. Detection of Rickettsia felis, Rickettsia typhi, Bartonella species and Yersinia pestis in fleas (Siphonaptera) from Africa. PLoS Neglected Tropical Diseases, 8, e3152.
- LEVIN, M. L., KILLMASTER, L. F. & ZEMTSOVA, G. E., 2012. Domestic dogs (Canis familiaris) as reservoir hosts for Rickettsia conorii. Vector-Borne and Zoonotic Diseases, 12, 28-33.
- LIDDELL, A. M., STOCKHAM, S. L., SCOTT, M. A., SUMNER, J. W., PADDOCK, C. D., GAUDREAULT-KEENER, M., ARENS, M. Q. & STORCH, G. A., 2003. Predominance of Ehrlichia ewingii in Missouri dogs. Journal of Clinical Microbiology, 41, 4617-4622.
- LIM, M. Y., BRADY, H., HAMBLING, T., SEXTON, K., TOMPKINS, D. & SLANEY, D., 2012. Rickettsia felis infections, New Zealand. Emerging Infectious Diseases, 18, 167-169.
- LIMA, M. L. F., SOARES, P. T., RAMOS, C. A. N., ARAÚJO, F. R., RAMOS, R. A. N., SOUZA, I. I. F., FAUSTINO, M. A. G. & ALVES, L. C. A., 2010. Molecular detection of Anaplasma platys in a naturally-infected cat in Brazil. Brazilian Journal of Microbiology, 41, 381-385.
- LITTLE, S. E. & HOWERTH, E. W., 1999. Ehrlichia chaffeensis in archived tissues of a white-tailed deer. Journal of Wildlife Diseases, 35, 596-599.
- LIU, Z., MA, M., WANG, Z., WANG, J., PENG, Y., LI, Y., GUAN, G., LUO, J. & YIN, H., 2012. Molecular survey and genetic identification of Anaplasma species in goats from central and southern China. Applied and Environmental Microbiology, 78, 464-470.
- LOFTIS, A. D., LEVIN, M. L. & SPURLOCK, J. P., 2008. Two USA Ehrlichia spp. cause febrile illness in goats. Veterinary Microbiology, 130, 398-402.
- LOFTIS, A. D., REEVES, W. K., SZUMLAS, D. E., ABBASSY, M. M., HELMY, I. M., MORIARITY, J. R. & DASCH, G. A., 2006. Surveillance of Egyptian fleas for agents of public health significance: Anaplasma, Bartonella, Coxiella, Ehrlichia, Rickettsia, and Yersinia pestis. American Journal of Tropical Medicine and Hygiene, 75, 41-48.
- LORUSSO, V., WIJNVELD, M., LATROFA, M. S., FAJINMI, A., MAJEKODUNMI, A. O., DOGO, A. G., IGWEH, A. C., OTRANTO, D., JONGEJAN, F., WELBURN, S. C. & PICOZZI, K., 2016. Canine and ovine tick-borne pathogens in camels, Nigeria. Veterinary Parasitology, 228, 90-92.
- LORUSSO, V., WIJNVELD, M., MAJEKODUNMI, A. O., DONGKUM, C., FAJINMI, A., DOGO, A. G., THRUSFIELD, M., MUGENYI, A., VAUMOURIN, E., IGWEH, A. C., JONGEJAN, F., WELBURN, S. C. & PICOZZI, K., 2016. Tick-borne pathogens of zoonotic and veterinary importance in Nigerian cattle. Parasites and Vectors, 9, 217.
- LOVRICH, S. D., JOBE, D. A., KOWALSKI, T. J., POLICEPATIL, S. M. & CALLISTER, S. M., 2011. Expansion of the Midwestern focus for human granulocytic anaplasmosis into the region surrounding La Crosse, Wisconsin. Journal of Clinical Microbiology, 05025-11.
- LUCE-FEDROW, A., MAINA, A. N., OTIANG, E., ADE, F., OMULO, S., OGOLA, E., OCHIENG, L., NJENGA, M. K. & RICHARDS, A. L., 2015. Isolation of Candidatus Rickettsia asemboensis from Ctenocephalides fleas. Vector-Borne and Zoonotic Diseases, 15, 268-277.
- M’GHIRBI, Y., BÈJI, M., OPORTO, B., KHROUF, F., HURTADO, A. & BOUATTOUR, A., 2016. Anaplasma marginale and A. phagocytophilum in cattle in Tunisia. Parasites and Vectors, 9, 556.
- M’GHIRBI, Y., GHORBEL, A., AMOURI, M., NEBAOUI, A., HADDAD, S. & BOUATTOUR, A., 2009. Clinical, serological, and molecular evidence of ehrlichiosis and anaplasmosis in dogs in Tunisia. Parasitology Research, 104, 767-774.
- M’GHIRBI, Y., YAÏCH, H., GHORBEL, A. & BOUATTOUR, A., 2012. Anaplasma phagocytophilum in horses and ticks in Tunisia. Parasites and Vectors, 5, 180.
- MACHADO, R. Z., M., T. M., C., R. A., R., A. M., R., G. L., DA SILVA, B. J. & PEREIRA, C. L., 2016. Molecular diagnosis and genetic diversity of tick-borne Anaplasmataceae agents infecting the African buffalo Syncerus caffer from Marromeu Reserve in Mozambique. Parasites and Vectors, 9, 454.
- MADEDDU, G., MANCINI, F., CADDEO, A., CIERVO, A., BABUDIERI, S., MAIDA, I., FIORI, M. L., REZZA, G. & MURA, M. S., 2012. Rickettsia monacensis as cause of Mediterranean spotted fever–like illness, Italy. Emerging Infectious Diseases, 18, 702.
- MAEDA, K., MARKOWITZ, N., HAWLEY, R. C., RISTIC, M., COX, D. & MCDADE, J. E., 1987. Human infection with Ehrlichia canis, a leukocytic rickettsia. New England Journal of Medicine, 316, 853-856.
- MAGGI, R. G., MASCARELLI, P. E., HAVENGA, L. N., NAIDOO, V. & BREITSCHWERDT, E. B., 2013. Co-infection with Anaplasma platys, Bartonella henselae and Candidatus Mycoplasma haematoparvum in a veterinarian. Parasites and Vectors, 6, 103.
- MAINA, A. N., JIANG, J., OMULO, S. A., CUTLER, S. J., ADE, F., OGOLA, E., FEIKIN, D. R., NJENGA, M. K., CLEAVELAND, S., MPOKE, S., NG'ANG'A, Z., BREIMAN, R. F., KNOBEL, D. L. & RICHARDS, A. L., 2014. High prevalence of Rickettsia africae variants in Amblyomma variegatum ticks from domestic mammals in rural western Kenya: implications for human health. Vector-Borne and Zoonotic Diseases, 14, 693-702.
- MAINA, A. N., LUCE-FEDROW, A., OMULO, S., HANG, J., CHAN, T. C., ADE, F., JIMA, D. D., OGOLA, E., GE, H., BREIMAN, R. F., NJENGA, M. K. & RICHARDS, A. L., 2016. Isolation and characterization of a novel Rickettsia species (Rickettsia asembonensis sp. nov.) obtained from cat fleas (Ctenocephalides felis). International Journal of Systematic and Evolutionary Microbiology, 66, 4512-4517.
- MAIOLI, G., PISTONE, D., BONILAURI, P., PAJORO, M., BARBIERI, I., MULATTO, P., VICARI, N. & DOTTORI, M., 2012. Ethiological agents of rickettsiosis and anaplasmosis in ticks collected in Emilia-Romagna region (Italy) during 2008 and 2009. Experimental and Applied Acarology, 57, 199-208.
- MARIÉ, J. L., SHAW, S., LANGTON, D., BOURRY, O., GOMEZ, J. & DAVOUST, B., 2009. Sub‐clinical infection of dogs from the Ivory Coast and Gabon with Ehrlichia, Anaplasma, Mycoplasma and Rickettsia species. Clinical Microbiology and Infection, 15, 284-285.
- MASALA, G., CHISU, V., FOXI, C., SOCOLOVSCHI, C., RAOULT, D. & PAROLA, P., 2012. First detection of Ehrlichia canis in Rhipicephalus bursa ticks in Sardinia, Italy. Ticks and Tick-Borne Diseases, 3, 396-397.
- MASSUNG, R. F., MAUEL, M. J., OWENS, J. H., ALLAN, N., COURTNEY, J. W., STAFFORD III, K. C. & MATHER , T. N., 2002. Genetic variants of Ehrlichia phagocytophila, Rhode island and Connecticut. Emerging Infectious Diseases, 8, 467.
- MASUZAWA, T., UCHISHIMA, Y., FUKUI, T., OKAMOTO, Y., PAN, M. J., KADOSAKA, T. & TAKADA, N., 2014. Detection of Anaplasma phagocytophilum and Anaplasma bovis in small wild mammals from Taichung and Kinmen Island, Taiwan. Japanese Journal of Infectious Diseases, 67, 111-114.
- MATEI, I. A., D'AMICO, G., YAO, P. K., IONICĂ, A. M., KANYARI, P. W., DASKALAKI, A. A., DUMITRACHE, M. O., SÁNDOR, A. D., GHERMAN, C. M., QABLAN, M., MODRÝ, D. & MIHALCA, A. D., 2016. Molecular detection of Anaplasma platys infection in free-roaming dogs and ticks from Kenya and Ivory Coast. Parasites and Vectors, 9, 157.
- MAURIN, M., BAKKEN, J. S. & DUMLER, J. S., 2003. Antibiotic susceptibilities of Anaplasma (Ehrlichia) phagocytophilum strains from various geographic areas in the United States. Antimicrobial Agents and Chemotherapy, 47, 413-415.
- MAXCY, K. F., 1926. An Epidemiological Study of Endemic Typhus (Brill's Disease) in the Southeastern United States: With Special Reference to Its Mode of Transmission. Public Health Reports (1896-1970), 2967-2995.
- MEDIANNIKOV, O., AUDOLY, G., DIATTA, G., TRAPE, J. F. & RAOULT, D., 2012. New< i> Rickettsia sp. in tsetse flies from Senegal. Comparative Immunology, Microbiology and Infectious Diseases, 35, 145-150.
- MEDIANNIKOV, O., DIATTA, G., FENOLLAR, F., SOKHNA, C., TRAPE, J. F. & RAOULT, D., 2010. Tick-borne rickettsioses, neglected emerging diseases in rural Senegal. PLoS Neglected Tropical Diseases, 4, e821.
- MEDIANNIKOV, O., DIATTA, G., ZOLIA, Y., BALDE, M. C., KOHAR, H., TRAPE, J. F. & RAOULT, D., 2012. Tick-borne rickettsiae in Guinea and Liberia. Ticks and Tick-Borne Diseases, 3, 43-48.
- MEDIANNIKOV, O., SOCOLOVSCHI, C., EDOUARD, S., FENOLLAR, F., MOUFFOK, N., BASSENE, H., DIATTA, G., TALL, A., NIANGALY, H., DOUMBO, O., LEKANA-DOUKI, J. B., ZNAZEN, A., SARIH, M., RATMANOV, P., RICHET, H., NDIATH, M. O., PAROLA, C. S. P. & RAOULT, D., 2013. Common epidemiology of Rickettsia felis infection and malaria, Africa. Emerging Infectious Diseases, 19, 1775.
- MERHEJ, V. & RAOULT, D., 2011. Rickettsial evolution in the light of comparative genomics. Biological Reviews, 86, 379-405.
- MINICHOVÁ, L., HAMSÍKOVÁ, Z., MAHRÍKOVÁ, L., SLOVÁK, M., KOCIANOVÁ, E., KAZIMÍROVÁ, M., SKULTÉTY, Ľ., STEFANIDESOVÁ, K. & SPITALSKÁ, E., 2017. Molecular evidence of Rickettsia spp. in ixodid ticks and rodents in suburban, natural and rural habitats in Slovakia. Parasites and Vectors, 10, 158.
- MOKRANI, K., TEBBAL, S., RAOULT, D. & FOURNIER, P. E., 2012. Human rickettsioses in the Batna area, eastern Algeria. Ticks and Tick-Borne Diseases, 3, 364-366.
- MOKRANI, N., PAROLA, P., TEBBAL, S., DALICHAOUCHE, M., AOUATI, A. & RAOULT, D., 2008. Rickettsia aeschlimannii infection, Algeria. Emerging Infectious Diseases, 14, 1814.
- MOUREMBOU, G., LEKANA-DOUKI, J. B., MEDIANNIKOV, O., NZONDO, S. M., KOUNA, L. C., ESSONE, J. C. B. B., FENOLLAR, F. & RAOULT, D., 2015. Possible role of Rickettsia felis in acute febrile illness among children in Gabon. Emerging Infectious Diseases, 21, 1808.
- MTSHALI, K., KHUMALO, Z. T., NAKAO, R., GRAB, D. J., SUGIMOTO, C. & THEKISOE, O. M., 2015. Molecular detection of zoonotic tick-borne pathogens from ticks collected from ruminants in four South African provinces. Journal of Veterinary Medical Science, 77, 1573-1579.
- MURA, A., SOCOLOVSCHI, C., GINESTA, J., LAFRANCE, B., MAGNAN, S., ROLAIN, J. M., DAVOUST, B., RAOULT, D. & PAROLA, P., 2008. Molecular detection of spotted fever group rickettsiae in ticks from Ethiopia and Chad. Transactions of the Royal Society of Tropical Medicine and Hygiene, 102, 945-949.
- MURPHY, G. L., EWING, S. A., WHITWORTH, L. C., FOX, J. C. & KOCAN, A. A., 1998. A molecular and serologic survey of Ehrlichia canis, E. chaffeensis, and E. ewingii in dogs and ticks from Oklahoma. Veterinary Parasitology, 79, 325-339.
- NAIR, A. S., RAVINDRAN, R., LAKSHMANAN, B., SREEKUMAR, C., KUMAR, S. S., RAJU, R., TRESAMOL, P. V., VIMALKUMAR, M. B. & SASEENDRANATH, M. R., 2013. Bovine carriers of Anaplasma marginale and Anaplasma bovis in South India. Tropical Biomedicine, 30, 105-112.
- NAKAO, R., QIU, Y., IGARASHI, M., MAGONA, J. W., ZHOU, L., ITO, K. & SUGIMOTO, C., 2013. High prevalence of spotted fever group rickettsiae in Amblyomma variegatum from Uganda and their identification using sizes of intergenic spacers. Ticks and Tick-Borne Diseases, 4, 506-512.
- NDIP, L. M., NDIP, R. N., ESEMU, S. N., WALKER, D. H. & MCBRIDE, J. W., 2010. Predominance of Ehrlichia chaffeensis in Rhipicephalus sanguineus ticks from kennel-confined dogs in Limbe, Cameroon. Experimental and Applied Acarology, 50, 163-168.
- NDIP, L. M., NDIP, R. N., NDIVE, V. E., AWUH, J. A., WALKER, D. H. & MCBRIDE, J. W., 2007. Ehrlichia species in Rhipicephalus sanguineus ticks in Cameroon. Vector-Borne and Zoonotic Diseases, 7, 221-227.
- NELDER, M. P., REEVES, W. K., ADLER, P. H., WOZNIAK, A. & WILLS, W., 2009. Ectoparasites and associated pathogens of free-roaming and captive animals in zoos of South Carolina. Vector-Borne and Zoonotic Diseases, 9, 469-477.
- NOAMAN, V. & SHAYAN, P., 2010. Molecular detection of Anaplasma bovis in cattle from central part of Iran, 1, 117-122. Presented at Veterinary Research Forum.
- NOGUERAS, M. M., PONS, I., ORTUÑO, A., MIRET, J., PLA, J., CASTELLÀ, J. & SEGURA, F., 2013. Molecular detection of Rickettsia typhi in cats and fleas. PLoS One, 8, e71386.
- NOWAK, M., CIENIUCH, S., STAŃCZAK, J. & SIUDA, K., 2010. Detection of Anaplasmaphagocytophilum in Amblyomma flavomaculatum ticks (Acari: Ixodidae) collected from lizard Varanus exanthematicus imported to Poland. Experimental and Applied Acarology, 51, 363-371.
- ODHIAMBO, A. M., MAINA, A. N., TAYLOR, M. L., JIANG, J. & RICHARDS, A. L., 2014. Development and Validation of a Quantitative Real-Time Polymerase Chain Reaction Assay Specific for the Detection of Rickettsia felis and Not Rickettsia felis-Like Organisms. Vector-Borne and Zoonotic Diseases, 7, 476-478.
- OGO, N. I., DE MERA, I. G., GALINDO, R. C., OKUBANJO, O. O., INUWA, H. M., AGBEDE, R. I., TORINA, A., ALONGI, A., VICENTE, J., GORTÁZAR, C. & DE LA FUENTE, J., 2012. Molecular identification of tick-borne pathogens in Nigerian ticks. Veterinary Parasitology, 187, 572-577.
- OHASHI, N., INAYOSHI, M., KITAMURA, K., KAWAMORI, F., KAWAGUCHI, D., NISHIMURA, Y., NAITOU, H., HIROI, M. & MASUZAWA, T., 2005. Anaplasma phagocytophilum–infected ticks, Japan. Emerging Infectious Diseases, 11, 1780.
- OMONDI, D., MASIGA, D. K., FIELDING, B. C., KARIUKI, E., AJAMMA, Y. U., MWAMUYE, M. M., OUSO, D. O. & VILLINGER, J., 2017. Molecular Detection of Tick-Borne Pathogen Diversities in Ticks from livestock and reptiles along the shores and adjacent islands of lake Victoria and lake Baringo, Kenya. Frontiers in Veterinary Science, 4, 73.
- ORTUÑO, A., PONS, I., QUESADA, M., LARIO, S., ANTON, E., GIL, A., CASTELLÀ, J. & SEGURA, F., 2012. Evaluation of the presence of Rickettsia slovaca infection in domestic ruminants in Catalonia, Northeastern Spain. Vector-Borne and Zoonotic Diseases, 12, 1019-1022.
- OSWE, M., ODHIAMBO, R., MUTAI, B., NYAKOE, N., AWINDA, G. & WAITUMBI, J. N., 2018. Zoonotic Pathogens in Ticks Collected from Livestock in Kenya. Open Journal of Preventive Medicine, 8, 248.
- PAROLA, P., DAVOUST, B. & RAOULT, D., 2005. Tick-and flea-borne rickettsial emerging zoonoses. Veterinary Research, 36, 469-492.
- PAROLA, P., INOKUMA, H., CAMICAS, J. L., BROUQUI, P. & RAOULT, D., 2001. Detection and identification of spotted fever group Rickettsiae and Ehrlichiae in African ticks. Emerging Infectious Diseases, 7, 1014-1018.
- PAROLA, P., PADDOCK, C. D. & RAOULT, D., 2005. Tick-borne rickettsioses around the world: emerging diseases challenging old concepts. Clinical Microbiology Reviews, 18, 719-756.
- PAROLA, P., PADDOCK, C. D., SOCOLOVSCHI, C., LABRUNA, M. B., MEDIANNIKOV, O., KERNIF, T., ABDAD, M. Y., STENOS, J., BITAM, I., FOURNIER, P. E. & RAOULT, D., 2013. Update on tick-borne rickettsioses around the world: a geographic approach. Clinical Microbiology Reviews, 26, 657-702.
- PAROLA, P., ROVERY, C., ROLAIN, J. M., BROUQUI, P., DAVOUST, B. & RAOULT, D., 2009. Rickettsia slovaca and R. raoultii in tick-borne rickettsioses. Emerging Infectious Diseases, 15, 1105.
- PAROLA, P., SANOGO, O. Y., LERDTHUSNEE, K., ZEAITER, Z., CHAUVANCY, G., GONZALEZ, J. P., MILLER, R. S., TELFORD III, S. R., WONGSRICHANALAI, C. & RAOULT, D., 2003. Identification of Rickettsia spp. and Bartonella spp. in Fleas from the Thai‐Myanmar Border. Annals of the New York Academy of Sciences, 990, 173-181.
- PAROLA, P., VESTRIS, G., MARTINEZ, D., BROCHIER, B., ROUX, V. & RAOULT, D., 1999. Tick-borne rickettiosis in Guadeloupe, the French West Indies: isolation of Rickettsia africae from Amblyomma variegatum ticks and serosurvey in humans, cattle, and goats. American Journal of Tropical Medicine and Hygiene, 60, 888-893.
- PAULAUSKAS, A., RADZIJEVSKAJA, J. & ROSEF, O., 2012. Molecular detection and characterization of Anaplasma phagocytophilum strains. Comparative Immunology, Microbiology and Infectious Diseases, 35, 187-195.
- PENNISI, M. G., CAPRÌ, A., SOLANO-GALLEGO, L., LOMBARDO, G., TORINA, A. & MASUCCI, M., 2012. Prevalence of antibodies against Rickettsia conorii, Babesia canis, Ehrlichia canis, and Anaplasma phagocytophilum antigens in dogs from the Stretto di Messina area (Italy). Ticks and Tick-Borne Diseases, 3, 315-318.
- POMPO, K., MAYS, S., WESSELMAN, C., PAULSEN, D. J. & FRYXELL, R. T., 2016. Survey of Ticks Collected from Tennessee Cattle and Their Pastures for Anaplasma and Ehrlichia Species. Journal of Parasitology, 102, 54-59.
- POPOV, V. L., HAN, V. C., CHEN, S. M., DUMLER, J. S., FENG, H. M., ANDREADIS, T. G., TESH, R. B. & WALKER, D. H., 1998. Ultrastructural differentiation of the genogroups in the genus Ehrlichia. Journal of Medical Microbiology, 47, 235-251.
- PRETORIUS, A. M. & BIRTLES, R. J., 2004. Rickettsia mongolotimonae infection in South Africa. Emerging Infectious Diseases, 10, 125.
- PRICE, J. E. & KARSTAD, L. H., 1980. Free-living jackals (Canis mesomelas)-potential reservoir hosts for Ehrlichia canis in Kenya. Journal of Wildlife Diseases, 16, 469-473.
- PSAROULAKI, A., GERMANAKIS, A., GIKAS, A., SCOULICA, E. & TSELENTIS, Y., 2005. Simultaneous detection of “Rickettsia mongolotimonae” in a patient and in a tick in Greece. Journal of Clinical Microbiology, 43, 3558-3559.
- RAOULT, D., BROUQUI, P. & ROUX, V., 1996. A new spotted-fever-group rickettsiosis. Lancet, 348, 412.
- RAOULT, D. & DRANCOURT, M., 1991. Antimicrobial therapy of rickettsial diseases. Antimicrobial Agents and Chemotherapy, 35, 2457.
- RAOULT, D., FOURNIER, P. E., ABBOUD, P. & CARON, F., 2002. First documented human Rickettsia aeschlimannii infection. Emerging Infectious Diseases, 8, 748.
- RAOULT, D., FOURNIER, P. E., EREMEEVA, M., GRAVES, S., KELLY, P. J., OTEO, J. A., SEKEYOVA, Z., TAMURA, A., TARASEVICH, I. & ZHANG, L., 2005. Naming of rickettsiae and rickettsial diseases. Annals of the New York Academy of Sciences, 1063, 1-12.
- RAOULT, D., FOURNIER, P. E., FENOLLAR, F., JENSENIUS, M., PRIOE, T., DE PINA, J. J., CARUSO, G., JONES, N., LAFERL, H., ROSENBLATT, J. E. & MARRIE, T. J., 2001. Rickettsia africae, a tick-borne pathogen in travelers to sub-Saharan Africa. New England Journal of Medicine, 344, 1504-1510.
- RAOULT, D., LAKOS, A., FENOLLAR, F., BEYTOUT, J., BROUQUI, P. & FOURNIER, P. E., 2002. Spotless rickettsiosis caused by Rickettsia slovaca and associated with Dermacentor ticks. Clinical Infectious Diseases, 34, 1331-1336.
- RAOULT, D. & PAROLA, P., 2007. Rickettsial diseases. New York: Informa Healthcare USA, Inc.
- RAR, V. & GOLOVLJOVA, I., 2011. Anaplasma, Ehrlichia, and “Candidatus Neoehrlichia” bacteria: pathogenicity, biodiversity, and molecular genetic characteristics, a review. Infection, Genetics and Evolution, 11, 1842-1861.
- RAR, V. A., LIVANOVA, N. N., PANOV, V. V., DOROSCHENKO, E. K., PUKHOVSKAYA, N. M., VYSOCHINA, N. P. & IVANOV, L. I., 2010. Genetic diversity of Anaplasma and Ehrlichia in the Asian part of Russia. Ticks and Tick-borne Diseases, 1, 57-65.
- RAVICINI, S., PASTOR, J., HAWLEY, J., BREWER, M., CASTRO-LÓPEZ, J., BEALL, M. & LAPPIN, M. R., 2016. Prevalence of selected infectious disease agents in stray cats in Catalonia, Spain. JFMS Open Reports, 2(1), 2055116916634109.
- RAVYN, M. D., KORENBERG, E. I., OEDING, J. A., KOVALEVSKII, Y. V. & JOHNSON, R. C., 1999. Monocytic Ehrlichia in Ixodes persulcatus ticks from Perm, Russia. Lancet, 722-723.
- REEVES, W. K., NELDER, M. P. & KORECKI, J. A., 2005. Bartonella and Rickettsia in fleas and lice from mammals in South Carolina, USA. Journal of Vector Ecology, 30, 310.
- REIF, K. E. & MACALUSO, K. R., 2009. Ecology of Rickettsia felis: a review. Journal of Medical Entomology, 46, 723-736.
- RENVOISE, A., JOLIOT, A. Y. & RAOULT, D., 2009. Rickettsia felis infection in man, France. Emerging Infectious Diseases, 15, 1126-1127.
- REYE, A. L., ARINOLA, O. G., HUBSCHEN, J. M. & MULLER, C. P., 2012. Pathogen prevalence in ticks collected from the vegetation and livestock in Nigeria. Applied and Environmental Microbiology, 78, 2562-2568.
- RICHARDS, A. L., JIANG, J., OMULO, S., DARE, R., ABDIRAHMAN, K., ALI, A., SHARIF, S. K., FEIKIN, D. R., BREIMAN, R. F. & K., N. M., 2010. Human infection with Rickettsia felis, Kenya. Emerging Infectious Diseases, 16, 1081.
- RIKIHISA, Y., 1991. The tribe Ehrlichieae and ehrlichial diseases. Clinical Microbiology Reviews, 4, 286-308.
- RJEIBI, M., AYADI, O., REKIK, M. & GHARBI, M., 2018. Molecular survey and genetic characterization of Anaplasma centrale, A. marginale and A. bovis in cattle from Algeria. Transboundary and Emerging Diseases, 65, 456-464.
- ROELLIG, D. M. & FANG, Q. Q., 2012. Detection of Anaplasma phagocytophilum in ixodid ticks from equine-inhabited sites in the Southeastern United States. Vector-Borne and Zoonotic Diseases, 12, 330-332.
- ROLAIN, J. M., BOURRY, O., DAVOUST, B. & RAOULT, D., 2005. Bartonella quintana and Rickettsia felis in Gabon. Emerging Infectious Diseases, 11, 1742.
- ROVERY, C. & RAOULT, D., 2008. Mediterranean spotted fever. Infectious Disease Clinics of North America, 22, 515-530.
- RYMASZEWSKA, A. & GRENDA, S., 2008. Bacteria of the genus Anaplasma–characteristics of Anaplasma and their vectors: a review. Veterinary Medicine, 53, 573-584.
- SAINZ, A., AMUSATEGUI, I. & TESOURO, M., 1999. Ehrlichia platys infection and disease in dogs in Spain. Journal of Veterinary Diagnostic Investigation, 11, 382-384.
- SAINZ, Á., ROURA, X., MIRÓ, G., ESTRADA-PEÑA, A., KOHN, B., HARRUS, S. & SOLANO-GALLEGO, L., 2015. Guideline for veterinary practitioners on canine ehrlichiosis and anaplasmosis in Europe. Parasites and Vectors, 8, 75.
- SAKAMOTO, L., ICHIKAWA, Y., SAKATA, Y., MATSUMOTO, K. & INOKUMA, H., 2010. Detection of Anaplasma bovis DNA in the peripheral blood of domestic dogs in Japan. Japanese Journal of Infectious Diseases, 63, 349-352.
- SALAKIJ, C., LERTWATCHARASARAKUL, P., SALAKIJ, J., NUNKLANG, K. & RATTANAKUNUPRAKARN, J., 2012. Molecular characterization of Anaplasma platys in a domestic cat from Thailand. Comparative Clinical Pathology, 21, 345-348.
- SAMBOU, M., FAYE, N., BASSÈNE, H., DIATTA, G., RAOULT, D. & MEDIANNIKOV, O., 2014. Identification of rickettsial pathogens in ixodid ticks in northern Senegal. Ticks and Tick-Borne Diseases, 5, 552-556.
- SANOGO, Y. I., PAROLA, P., SHPYNOV, S. N., CAMICAS, J. L., BROUQUI, P., CARUSO, G. & RAOULT, D., 2003. Genetic diversity of bacterial agents detected in ticks removed from asymptomatic patients in northeastern Italy. Annals of the New York Academy of Sciences, 990, 182-190.
- SANTOS, A. S., SANTOS-SILVA, M. M., ALMEIDA, V. C., BACELLAR, F. & DUMLER, J. S., 2004. Detection of Anaplasma phagocytophilum DNA in Ixodes ticks (Acari: Ixodidae) from Madeira island and Setubal district, mainland Portugal. Emerging Infectious Diseases, 10, 1643.
- SANTOS, C. & CARVALHO, C., 2006. First report of Anaplasma bovis (Donatien and Lestoquard, 1936) Dumler et al.(2001) at micro region of Campos dos Goytacazes, State of Rio de Janeiro, Brazil. Revista brasileira de parasitologia veterinaria = Brazilian Journal of Veterinary Parasitology: Orgao Oficial do Colegio Brasileiro de Parasitologia Veterinaria, 15, 126-127.
- SARIH, M., SOCOLOVSCHI, C., BOUDEBOUCH, N., HASSAR, M., RAOULT, D. & PAROLA, P., 2008. Spotted fever group rickettsiae in ticks, Morocco. Emerging Infectious Diseases, 14, 1067.
- SARIH, M. H., M'GHIRBI, Y., BOUATTOUR, A., GERN, L., BARANTON, G. & POSTIC, D., 2005. Detection and identification of Ehrlichia spp. in ticks collected in Tunisia and Morocco. Journal of Clinical Microbiology, 43, 1127-1132.
- SASAKI, H., ICHIKAWA, Y., SAKATA, Y., ENDO, Y., NISHIGAKI, K., MATSUMOTO, K. & INOKUMA, H., 2012. Molecular survey of Rickettsia, Ehrlichia, and Anaplasma infection of domestic cats in Japan. Ticks and Tick-Borne Diseases, 3, 308-311.
- SASHIKA, M., ABE, G., MATSUMOTO, K. & INOKUMA, H., 2011. Molecular survey of Anaplasma and Ehrlichia infections of feral raccoons (Procyon lotor) in Hokkaido, Japan. Vector-Borne and Zoonotic Diseases, 11, 349-354.
- SATTA, G., CHISU, V., CABRAS, P., FOIS, F. & MASALA, G., 2011. Pathogens and symbionts in ticks: a survey on tick species distribution and presence of tick-transmitted micro-organisms in Sardinia, Italy. Journal of Medical Microbiology, 60, 63-68.
- SCHMATZ, H., KRAUSS, H., VIERTEL, P., ISMAIL, A. & HUSSEIN, A., 1978. Seroepidemiological investigations in domestic ruminants from Egypt, Somalia and Jordan for the demonstration of complement fixing antibodies against Rickettsia and Chlamydia (author's transl). Acta Tropica, 35, 101-111.
- SELMI, M., MARTELLO, E., BERTOLOTTI, L., BISANZIO, D. & TOMASSONE, L., 2009. Rickettsia slovaca and Rickettsia raoultii in Dermacentor marginatus ticks collected on wild boars in Tuscany, Italy. Journal of Medical Entomology, 46, 1490-1493.
- SENG, P., SARIH, M., SOCOLOVSCHI, C., BOUDEBOUCH, N., HASSAR, M., PAROLA, P., RAOULT, D. & BROUQUI, P., 2009. Detection of Anaplasmataceae in ticks collected in Morocco. Clinical Microbiology and Infection 15, 86-87.
- SFAR, N., M'GHIRBI, Y., LETAIEF, A., PAROLA, P., BOUATTOUR, A. & RAOULT, D., 2008. First report of Rickettsia monacensis and Rickettsia helvetica from Tunisia. Annals of Tropical Medicine and Parasitology, 102, 561-564.
- SHIELDS, K., CUMMING, M., RIOS, J., WONG, M. T., ZWICKER, J. I., STRAMER, S. L. & ALONSO, C. D., 2015. Transfusion‐associated A naplasma phagocytophilum infection in a pregnant patient with thalassemia trait: a case report. Transfusion, 55, 719-725.
- SHPYNOV, S., FOURNIER, P. E., RUDAKOV, N., TARASEVICH, I. & RAOULT, D., 2006. Detection of members of the genera Rickettsia, Anaplasma, and Ehrlichia in ticks collected in the Asiatic part of Russia. Annals of the New York Academy of Sciences, 1078, 378-383.
- SILAGHI, C., SANTOS, A. S., JACINTO GOMES, J., CHRISTOVA, I., MATEI, I. A., WALDER, G., DOMINGOS, A., BELL-SAKYI, L., SPRONG, H., VON LOEWENICH, F. D., OTEO, J. A., DE LA FUENTE, J. & DUMLER, J. S., 2017. Guidelines for the direct detection of Anaplasma spp. in diagnosis and epidemiological studies. Vector-Borne and Zoonotic Diseases, 17, 12-22.
- SIMPSON, R., GAUNT, S., HAIR, J., KOCAN, K., HENK, W. & CASEY, H., 1991. Evaluation of Rhipicephalus sanguineus as a potential biologic vector of Ehrlichia platys. American Journal of Veterinary Research, 52, 1537-1541.
- SKOTARCZAK, B., 2003. Canine ehrlichiosis. Annals of Agricultural and Environmental Medicine, 10, 137-141.
- SOCOLOVSCHI, C., BARBAROT, S., LEFEBVRE, M., PAROLA, P. & RAOULT, D., 2010. Rickettsia sibirica mongolitimonae in traveler from Egypt. Emerging Infectious Diseases, 16, 1495.
- SOCOLOVSCHI, C., HUYNH, T., DAVOUST, B., GOMEZ, J., RAOULT, D. & PAROLA, P., 2009. Transovarial and trans‐stadial transmission of Rickettsiae africae in Amblyomma variegatum ticks. Clinical Microbiology and Infection, 15, 317-318.
- SOCOLOVSCHI, C., MATSUMOTO, K., MARIE, J. L., DAVOUST, B., RAOULT, D. & PAROLA, P., 2007. Identification of rickettsiae, Uganda and Djibouti. Emerging Infectious Diseases, 13, 1508.
- SOCOLOVSCHI, C., MEDIANNIKOV, O., SOKHNA, C., TALL, A., DIATTA, G., BASSENE, H., TRAPE, J. & RAOULT, D., 2010. Rickettsia felis–associated uneruptive fever, Senegal. Emerging Infectious Diseases, 16, 1140.
- SOCOLOVSCHI, C., PAGES, F., NDIATH, M. O., RATMANOV, P. & RAOULT, D., 2012. Rickettsia species in African Anopheles mosquitoes. PLoS One, 7, e48254.
- SOLANO-GALLEGO, L., KIDD, L., TROTTA, M., DI MARCO, M., CALDIN, M., FURLANELLO, T. & BREITSCHWERDT, E. B., 2006. Febrile illness associated with Rickettsia conorii infection in dogs from Sicily. Emerging Infectious Diseases, 12, 1985.
- SPARAGANO, O. A., DE VOS, A. P., PAOLETTI, B., CAMMÀ, C., DE SANTIS, P., OTRANTO, D. & GIANGASPERO, A., 2003. Molecular detection of Anaplasma platys in dogs using polymerase chain reaction and reverse line blot hybridization. Journal of Veterinary Diagnostic Investigation, 15, 527-534.
- SPITALSKA, E., BOLDIS, V., KOSTANOVA, Z., KOCIANOVA, E. & STEFANIDESOVA, K., 2008. Incidence of various tick-borne microorganisms in rodents and ticks of central Slovakia. Acta Virologica, 52, 175-179.
- SPITALSKÁ, E., STEFANIDESOVÁ, K., KOCIANOVÁ, E. & BOLDIS, V., 2012. Rickettsia slovaca and Rickettsia raoultii in Dermacentor marginatus and Dermacentor reticulatus ticks from Slovak Republic. Experimental and Applied Acarology, 57, 189-197.
- SPRONG, H., WIELINGA, P. R., FONVILLE, M., REUSKEN, C., BRANDENBURG, A. H., BORGSTEEDE, F., C., G. & VAN DER GIESSEN, J. W. B., 2009. Ixodes ricinus ticks are reservoir hosts for Rickettsia helvetica and potentially carry flea-borne Rickettsia species. Parasites and Vectors, 2, 41.
- SREEKUMAR, C., ANANDAN, R., BALASUNDARAM, S. & RAJAVELU, G., 1996. Morphology and staining characteristics of Ehrlichia bovis. Comparative Immunology, Microbiology and Infectious Diseases, 19, 79-83.
- STALEY, J. T., BOONE, D. R., BRENNER, D. J., DE VOS, P., GARRITY, G. M., GOODFELLOW, M., KRIEG, N. R., RAINEY, F. A. & SCHLEIFER, K., 2005. Bergey's Manual of Systematic Bacteriology. The Proteobacteria. New York, NY, UNITED STATES: Springer.
- STEIERT, J. G. & GILFOY, F., 2002. Infection rates of Amblyomma americanum and Dermacentor variabilis by Ehrlichia chaffeensis and Ehrlichia ewingii in southwest Missouri. Vector-Borne and Zoonotic Diseases, 2, 53-60.
- STUEN, S., 2016. Tick-Borne Fever (Anaplasma phagocytophilum Infection) in Sheep–A Review.
- STUEN, S., ARTURSSON, K. & OLSSON, E. E., 1998. Experimental infection of lambs with an equine granulocytic Ehrlichia species resembling the agent that causes human granulocytic ehrlichiosis (HGE). Acta Veterinaria Scandinavica, 39, 491-497.
- STUEN, S., GRANQUIST, E. G. & SILAGHI, C., 2013. Anaplasma phagocytophilum—a widespread multi-host pathogen with highly adaptive strategies. Frontiers in Cellular and Infection Microbiology, 3, 31.
- STUEN, S., MOUM, T., PETROVEC, M. & SCHOULS, L., 2006. Genetic variants of Anaplasma phagocytophilum in Norway. International Journal of Medical Microbiology, 296, 164-166.
- STUEN, S., NEVLAND, S. & MOUM, T., 2003. Fatal Cases of Tick‐Borne Fever (TBF) in Sheep Caused by Several 16S rRNA Gene Variants of Anaplasma phagocytophilum. Annals of the New York Academy of Sciences, 990, 433-434.
- TAMAMOTO, C., SEINO, N., SUZUKI, M., KAJI, K., TAKAHASHI, H. & INOKUMA, H., 2007. Detection of Ehrlichia muris DNA from sika deer (Cervus nippon yesoensis) in Hokkaido, Japan. Veterinary Parasitology, 150, 370-373.
- TESHALE, S., GEYSEN, D., AMENI, G., ASFAW, Y. & BERKVENS, D., 2015. Improved molecular detection of Ehrlichia and Anaplasma species applied to Amblyomma ticks collected from cattle and sheep in Ethiopia. Ticks and Tick-Borne Diseases, 6, 1-7.
- TIAN, Z. C., LIU, G. Y., SHEN, H., XIE, J. R., LUO, J. & TIAN, M. Y., 2012. First report on the occurrence of Rickettsia slovaca and Rickettsia raoultii in Dermacentor silvarum in China. Parasites and Vectors, 5, 19.
- TOMANOVIĆ, S., CHOCHLAKIS, D., RADULOVIĆ, Z., MILUTINOVIĆ, M., CAKIĆ, S., MIHALJICA, D., TSELENTIS, Y. & PSAROULAKI, A., 2013. Analysis of pathogen co-occurrence in host-seeking adult hard ticks from Serbia. Experimental and Applied Acarology, 59, 367-376.
- TOMASSONE, L., NUÑEZ, P., GÜRTLER, R. E., CEBALLOS, L. A., OROZCO, M. M., KITRON, U. D. & FARBER, M., 2008. Molecular detection of Ehrlichia chaffeensis in Amblyomma parvum ticks, Argentina. Emerging Infectious Diseases, 14, 1953-1955.
- TONNA, I., AZZOPARDI, C. M., PISCOPO, T., CUSCHIERI, P., FENOLLAR, F. & RAOULT, D., 2006. Characterisation of rickettsial diseases in a hospital-based population in Malta. Journal of Infection, 53, 394-402.
- UILENBERG, G., 1993. Other ehrlichioses of ruminants. In: WOLDEHEWIT, Z. & RISTIC, M., (eds). Rickettsial and Chlamydial diseases of Domestic Animals. Pergamon Press. 427.
- UILENBERG, G., 1993. Other ehrlichiosis of ruminants. Rickettsial and Chlamydial Ciseases of Comestic Animals. Pergamon Press, Oxford, United Kingdom, 269-279.
- VARELA-STOKES, A. S., 2007. Transmission of Ehrlichia chaffeensis from lone star ticks (Amblyomma americanum) to white-tailed deer (Odocoileus virginianus). Journal of Wildlife Diseases, 43, 376-381.
- VON LOEWENICH, F. D., BAUMGARTEN, B. U., SCHRÖPPEL, K., GEISSDÖRFE, W., RÖLLINGHOFF, M. & BOGDAN, C., 2003. High diversity of ankA sequences of Anaplasma phagocytophilum among Ixodes ricinus ticks in Germany. Journal of Clinical Microbiology, 41, 5033-5040.
- WALKER, D. H. & DUMLER, J. S., 1996. Emergence of the ehrlichioses as human health problems. Emerging Infectious Diseases, 2, 18.
- WALTER, G., BOTELHO-NEVERS, E., SOCOLOVSCHI, C., RAOULT, D. & PAROLA, P., 2012. Murine typhus in returned travelers: a report of thirty-two cases. American Journal of Tropical Medicine and Hygiene, 86, 1049-1053.
- WEN, B., CAO, W. & PAN, H., 2003. Ehrlichiae and ehrlichial diseases in china. Annals of the New York Academy of Sciences, 990, 45-53.
- WEN, B., RIKIHISA, Y., MOTT, J., FUERST, P. A., KAWAHARA, M. & SUTO, C., 1995. Ehrlichia muris sp. nov., identified on the basis of 16S rRNA base sequences and serological, morphological, and biological characteristics. International Journal of Systematic Bacteriology, 45, 250-254.
- WILLIAMS, M., IZZARD, L., GRAVES, S. R., STENOS, J. & KELLY, J. J., 2011. First probable Australian cases of human infection with Rickettsia felis (cat-flea typhus). Medical Journal of Australia, 194, 41-43.
- WOLDEHIWET, Z., 2010. The natural history of Anaplasma phagocytophilum. Veterinary Parasitology, 167, 108-122.
- WORMSER, G. P., DATTWYLER, R. J., SHAPIRO, E. D., HALPERIN, J. J., STEERE, A. C., KLEMPNER, M. S., KRAUSE, P. J., BAKKEN, J. S., STRLE, F., STANEK, G., BOCKENSTEDT, L., FISH, D., DUMLER, J. S. & NADELMAN, R. B., 2006. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clinical Infectious Diseases, 43, 1089-1134.
- WORTHINGTON, R. & BIGALKE, R., 2001. A review of the infectious disease of African wild ruminants. Onderstepoort Journal of Veterinary Research, 68, 291-323.
- YABSLEY, M. J., VARELA, A. S., TATE, C. M., DUGAN, V. G., STALLKNECHT, D. E., LITTLE, S. E. & DAVIDSON, W. R., 2002. Ehrlichia ewingii infection in white-tailed deer (Odocoileus virginianus). Emerging Infectious Diseases, 8, 668-671.
- YANG, J., LI, Y., LIU, Z., GUAN, G., CHEN, Z., LUO, J., WANG, X. & YIN, H., 2014. Molecular evidence for Anaplasma bovis infection in wild Reeves' muntjac (Muntiacus reevesi), southwest China. Journal of Wildlife Diseases, 50, 982-985.
- YBAÑEZ, A. P., MATSUMOTO, K., KISHIMOTO, T. & INOKUMA, H., 2012. Molecular analyses of a potentially novel Anaplasma species closely related to Anaplasma phagocytophilum detected in sika deer (Cervus nippon yesoensis) in Japan. Veterinary Microbiology, 157, 232-236.
- YBANEZ, A. P., SASHIKA, M. & INOKUMA, H., 2013. The phylogenetic position of Anaplasma bovis and inferences on the phylogeny of the genus Anaplasma. Journal of Veterinary Medical Science, 13, 0411.
- YOSHIKAWA, H., KIMURA, M., OGAWA, M., ROLAIN, J. M. & RAOULT, D., 2005. Laboratory-confirmed Mediterranean spotted fever in a Japanese traveler to Kenya. American Journal of Tropical Medicine and Hygiene, 73, 1086-1089.
- YOSHIMOTO, K., MATSUYAMA, Y., MATSUDA, H., SAKAMOTO, L., MATSUMOTO, K., YOKOYAMA, N. & INOKUMA, H., 2010. Detection of Anaplasma bovis and Anaplasma phagocytophilum DNA from Haemaphysalis megaspinosa in Hokkaido, Japan. Veterinary Parasitology, 168, 170-172.
- ZEIDNER, N. S., BURKOT, T. R., MASSUNG, R., NICHOLSON, W. L., DOLAN, M. C., RUTHERFORD, J. S., BIGGERSTAFF, B. J. & MAUPIN, G. O., 2000. Transmission of the agent of human granulocytic ehrlichiosis by Ixodes spinipalpis ticks: evidence of an enzootic cycle of dual infection with Borrelia burgdorferi in Northern Colorado. Journal of Infectious Diseases, 182, 616-619.
- ZEMTSOVA, G., KILLMASTER, L., MUMCUOGLU, K. & LEVIN, M. L., 2010. Co-feeding as a route for transmission of Rickettsia conorii israelensis between Rhipicephalus sanguineus ticks. Experimental and Applied Acarology, 52, 383-392.
- ZEROUAL, F., LEULMI, H., BITAM, I. & BENAKHLA, A., 2018. Molecular evidence of Rickettsia slovaca in spleen of wild boars in northeastern Algeria. New Microbes and New Infections, 24, 17-20.
- ZHANG, H., CHANG, Z., MEHMOOD, K., WANG, Y., REHMAN, M. U., NABI, F., SABIR, A. J., LIU, X., WU, X., TIAN, X. & ZHOU, D., 2017. First report of Ehrlichia infection in goats, China. Microbial Pathogenesis, 110, 275-278.
- ZHANG, X. F., ZHANG, J. Z., LONG, S. W., RUBLE, R. P. & YU, X. J., 2003. Experimental Ehrlichia chaffeensis infection in beagles. Journal of Medical Microbiology, 52, 1021-1026.
- ZNAZEN, A., SELLAMI, H., ELLEUCH, E., HATTAB, Z., SASSI, L. B., KHROUF, F., DAMMAK, H., LETAIEF, A., JEMAA, M. B. & HAMMAMI, A., 2015. Comparison of two quantitative real time PCR assays for Rickettsia detection in patients from Tunisia. PLoS Neglected Tropical Diseases, 9, e0003487.




